Not long ago, a doctor’s appointment meant driving to a clinic, waiting in a crowded room, and spending 10 minutes with a physician who had already seen 40 patients that day. That model is being quietly dismantled, and AI is leading the charge.
In 2026, telemedicine is no longer just “video calls with doctors.” It is an intelligent, data-aware healthcare ecosystem where AI triages patients before a doctor even logs in, where remote sensors alert care teams about a diabetic patient’s blood sugar spike at 3 AM, and where natural language models write clinical notes while the physician focuses entirely on the patient.
The numbers tell the story clearly. The global telemedicine market, valued at $111.99 billion in 2025, is projected to surpass $532 billion by 2034 at a 20% CAGR. In India alone, the market is expected to grow from $3.64 billion in 2025 to $12.63 billion by 2031, driven by 820 million internet users, surging smartphone penetration, and government initiatives like eSanjeevani and Ayushman Bharat Digital Mission.
And at the heart of this transformation? AI.
If you are a healthcare startup, a hospital system, or a product company planning to build or upgrade a telemedicine platform in 2026, this guide is for you. We will cover everything, from how AI is reshaping virtual care to what features you need, how compliance works, what it costs, and what your competitors are missing.
Table of Contents
The State of Telemedicine in 2026: Why “Just Video Calls” Is Dead
From Convenience Feature to Core Infrastructure
When telemedicine first went mainstream during the pandemic, most platforms were digital wrappers around video conferencing. A calendar, a video link, a prescription PDF. That was enough then.
In 2026, that baseline no longer clears the bar for market entry. The top telehealth platforms launching today are deeply integrated into clinical workflows, pulling data from EHRs, processing wearable inputs in real time, and using AI to assist every step of the care journey, from the moment a patient types their first symptom.
As one recent industry analysis put it: the bar for a “telemedicine app” in 2026 is a tightly integrated, data-aware workflow that can stand up in front of clinicians, payers, and regulators, not a side experiment that lives in its own analytics island.
The AI Telemedicine Market: Scale and Speed
The AI-dedicated telehealth market is projected to grow from $4.22 billion in 2024 to $27.14 billion by 2030, a staggering 36.4% compound annual growth rate. The primary drivers: AI-powered intake automation, symptom triage, clinical documentation assistance, and patient engagement tools.
In India specifically, around 60% of telemedicine providers now utilize AI-driven tools to streamline operations, a number that has grown sharply over the last 18 months.
This is no longer a trend to watch. It is a market to build for.
How AI Is Transforming Telemedicine: 8 Core Use Cases
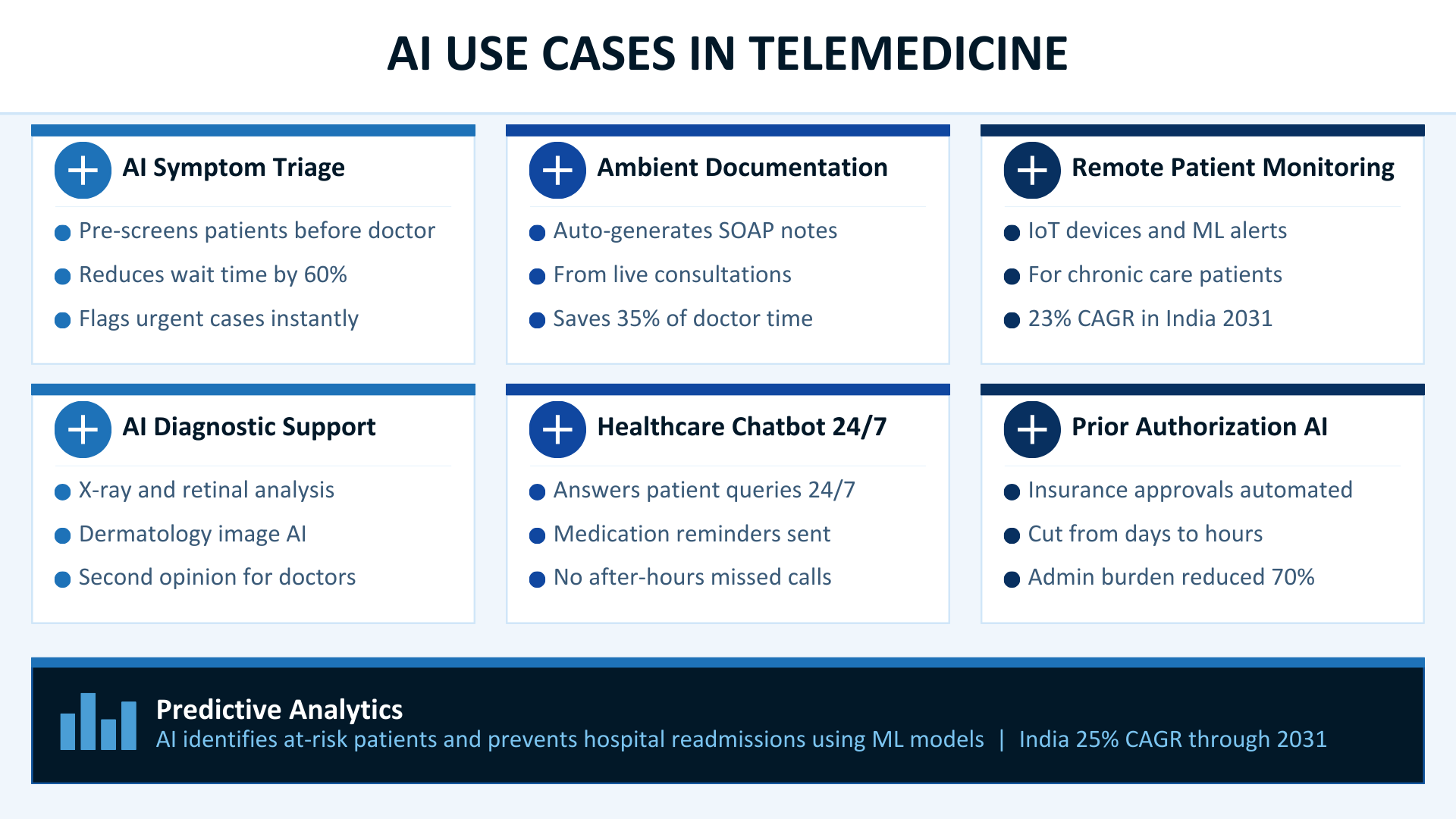

AI-Powered Symptom Triage (Before the Doctor Joins)
Traditional telemedicine: Patient joins, waits, then describes symptoms to a doctor in real time.
AI-powered telemedicine: Before the appointment even begins, an AI triage engine collects the patient’s symptoms, cross-references them with their medical history, flags urgent cases, assigns severity scores, and routes the patient to the appropriate specialist, all in under 90 seconds.
This is not speculative. Platforms like Ada Health and Buoy have demonstrated that AI symptom checkers can match physician triage accuracy in many primary care scenarios. For developers building in 2026, this functionality has moved from “advanced feature” to expected baseline for any serious platform entering the market.
For Webkorps clients: We build custom AI triage engines that integrate directly with your patient intake workflows, reducing average pre-consultation time by up to 60%.
Ambient Clinical Documentation (The End of Note-Taking)
One of the biggest pain points in telemedicine? Documentation.
Physicians spend an estimated 35-40% of their working time on administrative tasks, much of it writing or dictating clinical notes after consultations. AI ambient listening technology, where an AI model sits in the background of a video consultation, transcribes the conversation, and auto-generates structured SOAP notes, prescriptions, and follow-up instructions, is now production-ready and HIPAA-compliant.
Companies like Abridge and Nuance DAX (Microsoft) have already deployed this at scale in major US health systems. In 2026, building a telemedicine platform without ambient documentation support means your doctors will choose a competitor’s tool over yours.
Key technical consideration: Ambient AI transcription must use de-identified data pipelines, and clinical notes must remain in-platform or in the integrated EHR, never in third-party servers without a Business Associate Agreement (BAA).
Remote Patient Monitoring (RPM) with AI Alerts
AI-powered RPM connects smart devices, blood pressure cuffs, glucose monitors, ECG patches, pulse oximeters, to your telemedicine platform and runs machine learning algorithms over the incoming data stream in real time.
The result: instead of discovering a patient’s deteriorating condition at their next scheduled appointment, your platform alerts the care team the moment a biomarker crosses a threshold or even before, using predictive models trained on thousands of similar patient histories.
For chronic disease management, diabetes, hypertension, COPD, and heart failure, this is transformative. It is also the fastest-growing segment in the Indian telemedicine market, with home-care users showing a 23.12% CAGR through 2031.
What most platforms miss: True RPM is not just data collection. It is contextual AI analysis. A single elevated blood pressure reading is noise. Three elevated readings over 48 hours, combined with a patient’s reported headache in their daily check-in, is a signal. Your AI layer needs to understand the difference.
AI Diagnostic Support for Physicians
AI diagnostic tools analyze medical images, X-rays, retinal scans, dermatology photographs, and ECG waveforms during or before telemedicine consultations and surface preliminary findings for physician review.
This is not about replacing doctors. It is about giving them a second pair of eyes that has processed millions of cases and flags what might be easy to miss at the end of a 12-hour shift.
In India, where the doctor-to-patient ratio remains a persistent challenge (approximately 1 doctor per 834 patients in rural areas), AI diagnostic support is not a luxury; it is a force multiplier.
Personalized Treatment Plans Using Predictive Analytics
Using a patient’s historical data, genetic markers (where available), medication history, and real-world outcomes from similar patient profiles, AI can help physicians generate and refine personalized treatment plans rather than relying purely on general clinical guidelines.
Predictive analytics can also identify which patients are at high risk of hospital readmission, allowing care teams to intervene proactively with follow-up calls, medication adjustments, or remote check-ins.
AI Chatbots for 24/7 Patient Engagement
Between consultations, patients have questions. Most of those questions do not require a physician. They need reliable, empathetic, medically accurate responses at 11 PM, when no clinic is open.
AI-powered healthcare chatbots handle appointment scheduling, medication reminders, symptom follow-ups, lab result explanations, and post-discharge care instructions. Done well, they dramatically reduce call center volume and improve patient satisfaction scores.
What separates good from bad: A healthcare chatbot that confidently gives wrong medical information is dangerous. Guardrails, clinical content review, and clear escalation paths to human staff are non-negotiable.
AI-Powered Mental Health Support
Mental health represents one of the fastest-growing telemedicine segments globally, and one of the most AI-amenable. The Indian mental health telemedicine market is projected to grow at 25.55% CAGR through 2031.
AI tools in mental health telemedicine include mood tracking, CBT-based digital therapeutics, voice analysis for depression indicators, and AI-moderated group therapy session facilitation. The key design challenge: these tools must be clinically validated, ethically designed, and must always provide clear pathways to human professional support.
Insurance Verification and Prior Authorization Automation
One of the most overlooked AI use cases in telemedicine: automating the administrative nightmare of insurance verification and prior authorization.
An AI layer that checks real-time eligibility, predicts approval likelihood, and auto-generates prior authorization documentation can reduce the average authorization turnaround from days to hours, and dramatically improve physician and patient experience.
Must-Have Features for an AI-Powered Telemedicine Platform in 2026
Core Features (Non-Negotiable)
Every production-ready telemedicine platform in 2026 needs:
- HIPAA-compliant video consultation with sub-500ms latency on standard 4G connections
- Intelligent appointment scheduling with AI-based slot optimization and no-show prediction
- Secure, encrypted messaging between patients and care teams
- EHR/EMR integration via FHIR APIs (Epic, Cerner, or custom hospital systems)
- E-prescription with pharmacy routing via Surescripts or equivalent
- Multi-role access for patients, physicians, nurses, and administrative staff
- AI symptom triage before consultations
- Audit trails for every data interaction (required for HIPAA compliance)
Advanced Features (Competitive Differentiation)
- Ambient AI clinical documentation (SOAP note generation from voice)
- Remote patient monitoring with IoT device integrations
- AI diagnostic image analysis (X-rays, dermatology, retinal scans)
- Wearable device sync (Apple Health, Google Fit, medical-grade monitors)
- Voice-enabled AI assistant for elderly or low-literacy users
- Multilingual support with real-time AI translation (critical for India’s linguistic diversity)
- Predictive analytics dashboard for care team oversight
- Insurance verification and prior authorization automation
India-Specific Features (Unique Opportunity)
Most telemedicine platforms built by global companies are designed primarily for the US or European market. This creates a significant opening for India-based development companies like Webkorps:
- ABDM (Ayushman Bharat Digital Mission) integration for ABHA health ID linking
- eSanjeevani API compatibility for government healthcare initiatives
- Low-bandwidth video optimization for Tier-2 and Tier-3 city connectivity
- UPI and regional payment gateway integration for seamless billing
- Regional language voice input (Hindi, Tamil, Telugu, Bengali, and others)
- DPDP Act compliance (India’s Digital Personal Data Protection Act)
Compliance: HIPAA, DPDP, and What You Cannot Afford to Skip
Why Compliance Must Be Built In, Not Bolted On
The average cost of a healthcare data breach reached $7.42 million in 2025. In India, non-compliance with DPDP Act provisions can result in fines of up to INR 250 crore. Compliance is not a checkbox; it is your platform’s foundation.
HIPAA Compliance for Telemedicine (US Market)
If you are building for the US market or handling data from US patients:
Technical Safeguards Required:
- End-to-end encryption for all video, audio, messages, and files (TLS 1.2 minimum, AES-256 at rest)
- Role-based access control (RBAC), no user should access data outside their clinical role
- Multi-factor authentication for all provider accounts
- Automatic logoff after inactivity periods
- Audit logs for every PHI interaction
- Encrypted video codecs (VP9, H.264)
Administrative Requirements:
- Business Associate Agreements (BAAs) with every third-party vendor that touches PHI, including your video API provider, cloud storage, transcription service, and AI model provider
- HIPAA Security Risk Assessment before launch and annually thereafter
- Incident response and breach notification protocols
Critical Note on AI APIs: If you are using OpenAI, Google, or Anthropic APIs for AI features in your platform, you must ensure they have signed a BAA and that PHI is not used for model training. OpenAI now offers HIPAA-eligible configurations under its healthcare program. Verify this for every AI component in your stack.
India Compliance: DPDP Act 2023
India’s Digital Personal Data Protection Act imposes specific requirements on healthcare platforms:
- Explicit consent before collecting any health data
- Data localization mandates: patient data must be stored on servers within India
- Clear purpose limitation: Data collected for telemedicine cannot be repurposed for advertising
- Mandatory breach notification to CERT-In within 6 hours of discovery
HL7 FHIR: The Standard You Cannot Ignore
FHIR (Fast Healthcare Interoperability Resources) is now the de facto standard for healthcare data exchange. Any serious telemedicine platform must be FHIR R4 compliant to integrate with hospitals’ EHR systems. Skipping FHIR compliance means manual data entry, which means physician frustration, which means your platform will not get adopted.
Also read: HIPAA-Compliant AI Software Development: The Complete Guide for Healthcare Companies in 2026
The Tech Stack for an AI-Powered Telemedicine Platform in 2026
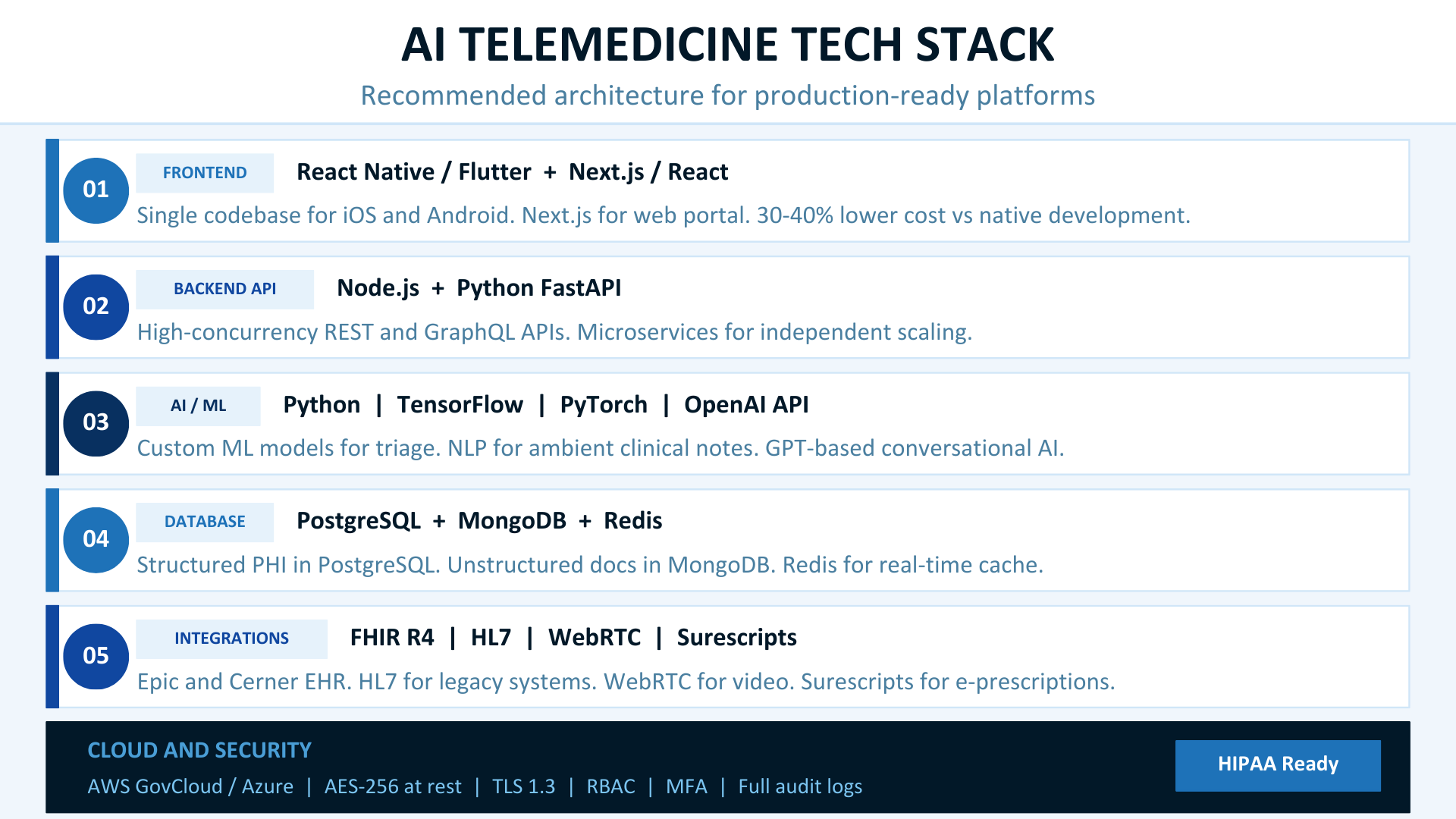
| Layer | Recommended Technology | Why |
|---|---|---|
| Frontend (Mobile) | React Native / Flutter | Single codebase for iOS and Android; 30-40% cost reduction vs. native |
| Frontend (Web) | React.js / Next.js | SEO-friendly, fast rendering, large talent pool |
| Backend | Node.js / Python (FastAPI) | High concurrency for real-time features; Python for AI/ML integration |
| Video Infrastructure | WebRTC + Twilio / LiveKit | Sub-500ms latency; HIPAA-compliant configurations available |
| AI/ML | Python, TensorFlow / PyTorch, OpenAI API | Production-grade ML; GPT-based clinical NLP |
| Database | PostgreSQL + MongoDB | Structured clinical data + flexible document storage |
| EHR Integration | FHIR R4 APIs | Epic, Cerner, Athenahealth interoperability |
| Cloud Infrastructure | AWS (GovCloud) / Azure (HIPAA-eligible) | Pre-built HIPAA compliance tooling; BAA available |
| Wearable/IoT | Apple HealthKit, Google Fit, MQTT protocol | Standard consumer + medical device connectivity |
| Security | AES-256, SSL/TLS 1.3, OWASP guidelines | Regulatory compliance + data protection |
A note on video infrastructure: WebRTC is the standard for real-time video, but implementing it correctly for telemedicine, handling poor network conditions, fallback protocols, latency on rural 4G networks, and HIPAA-compliant recording, requires deep expertise. This is where most DIY builds fail.
How to Build an AI Telemedicine Platform: Step-by-Step Process
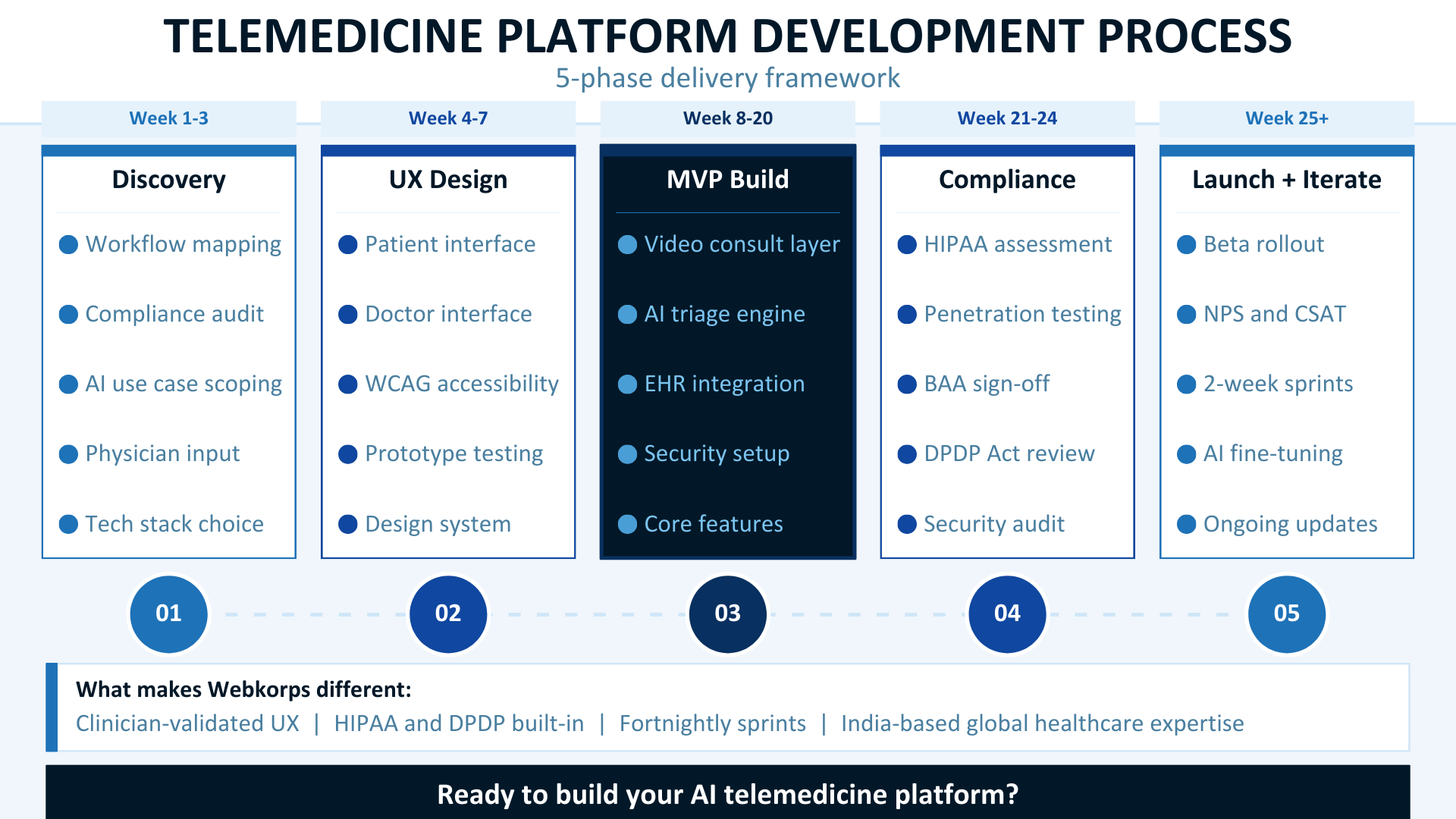
Phase 1: Discovery and Strategy (Weeks 1-3)
This is the phase most teams skip or rush, and it is the most expensive mistake you can make.
During discovery, you need to:
- Define your target user personas (patient demographics, provider types, payer relationships)
- Map clinical workflows with input from actual physicians and nurses
- Identify which AI use cases deliver the highest ROI for your specific market
- Conduct HIPAA/DPDP compliance assessment
- Define integration requirements (which EHR systems do your target hospitals use?)
- Prioritize MVP feature set based on clinical value, not engineering preference
What most teams miss: Involving clinicians in UX design from day one. Doctor-facing interfaces built without clinical input consistently fail adoption, and physician adoption is the single most important predictor of telemedicine platform success.
Phase 2: UI/UX Design (Weeks 4-7)
Healthcare UX has unique requirements:
- Zero-friction onboarding for elderly patients (large text, simple navigation, voice input)
- Dual-interface design – patient experience and physician experience are radically different
- Accessibility compliance (WCAG 2.1 AA) – required for healthcare applications
- Trust signals at every step: clear data privacy notices, verification badges for physicians
Phase 3: MVP Development (Weeks 8-20)
For a solid MVP covering core features (video consultation, scheduling, secure messaging, basic EHR integration, and AI triage), expect:
- 12-20 weeks of development with an experienced healthcare team
- 3-5 months for platforms including RPM, ambient documentation, and wearable integration
MVP-first is the right strategy. Launching a focused MVP with 50-200 beta users and iterating based on real clinical feedback is consistently better than building everything at once. It reduces initial costs by 40-60% and dramatically improves adoption outcomes.
Phase 4: Compliance and Security Testing
This phase is non-negotiable and often underscoped:
- HIPAA risk assessment: $4,000-$50,000 depending on platform complexity
- Penetration testing by a qualified healthcare security firm
- FHIR integration testing with actual EHR sandbox environments
- BAA execution with all third-party service providers
Phase 5: Soft Launch and Iteration
Launch with a beta cohort. Track:
- Video call quality (MOS scores, connection failure rates by device and network type)
- Appointment completion rates vs. in-person baseline
- Physician time spent per consultation (AI documentation should reduce this)
- Patient satisfaction scores (CSAT/NPS)
- No-show rates
The most successful telemedicine platforms ship meaningful feature updates every two weeks based on clinical user feedback. Build this iteration cadence into your roadmap from day one.
Telemedicine App Development Cost in 2026: Honest Numbers

| Platform Type | Timeline | Cost Range |
|---|---|---|
| Basic MVP (video, scheduling, messaging, e-prescription) | 3-5 months | $40,000 – $80,000 |
| Mid-Level (EHR integration, AI triage, patient portal) | 5-9 months | $80,000 – $180,000 |
| Advanced (RPM, ambient AI, wearables, multi-provider) | 9-18 months | $180,000 – $350,000 |
| Enterprise (multi-location, custom AI models, complex integrations) | 12-24 months | $350,000+ |
Key Cost Drivers
EHR Integration: A single Epic or Cerner integration adds $15,000-$35,000. Multiple system integrations can add $40,000-$100,000. This is not optional for hospital-facing platforms.
AI Features: Adding AI symptom triage and basic chatbot functionality adds $15,000-$35,000. Custom ML models trained on your specific patient population can add $50,000-$150,000.
HIPAA Compliance Implementation: Security architecture, audit systems, encryption, and compliance testing: $10,000-$30,000 on top of development costs.
India Advantage: Development teams in India, including Webkorps, offer production-quality healthcare software development at significantly lower rates than US or European agencies, without compromising on compliance expertise or clinical domain knowledge. This makes India the strategic choice for healthcare startups globally looking to build serious telemedicine infrastructure.
The Hidden Cost Most Builders Ignore: Post-Launch
A launched telemedicine platform is not a finished product. Budget for:
- Monthly cloud infrastructure: $2,000-$15,000 depending on scale
- Ongoing security monitoring and updates: $1,500-$5,000/month
- Annual HIPAA risk assessment: $5,000-$15,000
- Feature development iteration: plan for 20-30% of initial build cost annually
The Future of AI in Telemedicine: What’s Coming in 2027 and Beyond
Agentic AI in Healthcare
The next frontier is not AI that assists, it is AI that acts. Agentic AI in healthcare systems that can autonomously schedule follow-up appointments, refill standard prescriptions, coordinate between specialists, and manage care pathways for chronic conditions are already in early deployment at leading health systems.
AR/VR in Virtual Care
From virtual physiotherapy sessions to immersive psychiatric treatment environments, spatial computing is making virtual care feel less like a video call and more like a clinical encounter. Platforms building AR/VR capabilities today will have a significant advantage in 2027.
Predictive Population Health Management
AI that monitors population-level data to predict disease outbreaks before they occur, analyzing environmental data, mobility patterns, and social determinants, is becoming a standard expectation from government health systems. This is a significant contract opportunity for platforms with robust data infrastructure.
Blockchain for Health Data Sovereignty
Patient-controlled health records using blockchain, where a patient owns their health data and grants access to providers on demand, is moving from concept to early implementation. India’s Ayushman Bharat Digital Mission is laying the foundational infrastructure for this.
Why Choose Webkorps for Your Telemedicine Platform
Building an AI-powered telemedicine platform requires three things that most development teams cannot offer together: deep healthcare domain knowledge, enterprise-grade AI development capabilities, and rigorous compliance expertise.
At Webkorps, we have built healthcare software that serves patients across India and internationally. Our telemedicine development practice covers:
- End-to-end platform development: from UX design through AI integration, EHR connectivity, and compliance validation
- HIPAA and DPDP Act compliance: built into architecture from day one, not retrofitted after launch
- AI feature development: custom symptom triage, ambient documentation, RPM analytics, and diagnostic support tools
- India-specific optimization: ABDM integration, multilingual support, low-bandwidth video, and UPI payment connectivity
- Ongoing partnership: we do not hand off and disappear; we iterate with you based on clinical user feedback
Whether you are a healthcare startup building your first MVP or a hospital system modernizing legacy infrastructure, we would like to understand your specific challenges.
Get a free telemedicine platform consultation
Conclusion
The telemedicine industry in 2026 is not waiting for anyone to catch up.
AI is not a future feature for virtual care platforms; it is the present expectation. Patients expect intelligent triage before they speak to a doctor. Physicians expect their documentation to write itself. Care teams expect real-time alerts when a patient’s condition changes, not a report at the next appointment.
Building a smart virtual care platform in 2026 means building one where AI is woven into the architecture from the beginning, not added as an afterthought when a competitor forces your hand.
For India-based healthcare entrepreneurs and global startups building for India’s $4.97 billion telemedicine market, the opportunity is exceptional. The combination of government-mandated digital health infrastructure (ABDM, eSanjeevani), a massive underserved population in Tier-2 and Tier-3 cities, and world-class development capability at competitive costs makes this the right market, at the right moment.
The question is not whether to build. It is about how to build it right.
Ready to build your AI telemedicine platform? Talk to Webkorps, we have the healthcare domain expertise, AI development capabilities, and compliance knowledge to make it real.
Frequently Asked Questions
How much does it cost to build an AI telemedicine app in India?
A production-ready MVP with core features (video, scheduling, AI triage, EHR integration) typically costs $40,000-$80,000 when built by an experienced Indian development team. Advanced platforms with full AI features can range from $150,000-$350,000. India offers significantly better value than US or European agencies for the same quality of output.
How long does it take to build a telemedicine platform?
A focused MVP takes 3-5 months. Platforms with EHR integrations, AI features, and RPM capability typically require 6-9 months. Enterprise-grade multi-provider systems can take 12-18 months. The correct timeline depends heavily on your specific feature requirements and the complexity of your compliance environment.
What is the difference between HIPAA compliance and DPDP Act compliance?
HIPAA (US law) governs the handling of Protected Health Information (PHI) for US patients and providers. India’s Digital Personal Data Protection (DPDP) Act governs personal data handling in India, with specific data localization requirements and consent mandates. If you are building for both markets, both frameworks must be addressed simultaneously in your architecture.
Can AI replace doctors in telemedicine?
No, and this is an important distinction. AI in telemedicine is designed to augment physician capabilities, not replace clinical judgment. AI handles triage, documentation, data analysis, and administrative automation so that physicians can focus entirely on the clinical interaction. The physician remains the final authority on diagnosis and treatment.
What AI features should I prioritize in my telemedicine MVP?
For most markets, the highest-ROI AI features for an MVP are:
- AI symptom triage before consultations
- AI-assisted appointment scheduling with no-show prediction
- Automated clinical note generation.
These three features reduce administrative burden for providers, improve patient throughput, and are achievable within reasonable MVP budgets.
Is eSanjeevani integration important for telemedicine platforms in India?
If you are targeting the Indian government healthcare market or rural patients, eSanjeevani compatibility is strategically important. It gives your platform access to India’s national telemedicine infrastructure and a built-in patient base. For private healthcare, ABDM/ABHA integration is the more commercially relevant priority.

