Picture this: a patient is discharged after knee replacement surgery. No care coordinator scrambles to book the follow-up. No reminder slips through the cracks three days later. No prior authorization request sits in a queue for 11 days while the patient waits to start physical therapy. Instead, an autonomous AI agent has already scheduled the follow-up appointment, confirmed insurance eligibility, ordered the physical therapy referral, sent personalized pre-visit instructions in plain language, flagged a potential drug interaction in the discharge medications, and transmitted the complete surgical record to the receiving rehabilitation center – all before the patient reaches the hospital parking lot. This is not science fiction. This is agentic AI in healthcare, and it is already live in production at health systems across the United States.
Healthcare has historically been a reactive industry. Patients fall through the gaps between discharge and follow-up. Care coordinators are overwhelmed managing dozens of simultaneous transitions. Administrative tasks consume approximately 20 percent of institutional budgets, and physicians spend up to 25 percent of their working hours on non-clinical duties that contribute nothing to patient outcomes. The system is not broken because clinicians are bad at their jobs – it is broken because human coordination at scale is structurally impossible.
Agentic AI – systems capable of autonomous reasoning, planning, and multi-step task execution with defined human oversight – is shifting that structural reality. Unlike passive AI tools that wait for a prompt, agentic systems receive a goal, decompose it into tasks, act across multiple clinical and administrative systems simultaneously, and adapt their approach based on real-time outcomes. They do not just generate content. They take action.
KEY MARKET SIGNAL
61% of healthcare leaders are already building or have budgeted agentic AI initiatives, and 85% expect it to deliver moderate-to-significant value across clinical, business, and back-office functions in 2026. (Deloitte US Health Care Outlook, 2026)
This guide provides a comprehensive, practical breakdown of what agentic AI actually is in a healthcare context, how it manages patient journeys end-to-end through every stage of care, which health systems are already deploying it at scale, what the quantified benefits look like, which risks must be addressed proactively, what governance frameworks are required, and how to start building today. If you are a healthcare technology leader, CIO, CMO, or digital transformation executive, this is the article that should shape your next 12 months of investment thinking.
Table of Contents
Agentic AI vs. Traditional Healthcare AI – What’s Actually Different?
Before exploring how agentic AI transforms the patient journey, it is essential to understand exactly what makes it different from everything that came before it. The word ‘agentic’ is rapidly becoming one of the most overused terms in healthcare technology – vendors are applying it to everything from simple chatbots to basic robotic process automation. Understanding the genuine distinction is not just semantic. It determines whether your investment will produce transformative outcomes or expensive disappointment.
The Three Generations of AI in Healthcare
Healthcare AI has evolved through three distinct generations, each representing a qualitative leap in capability and autonomy:
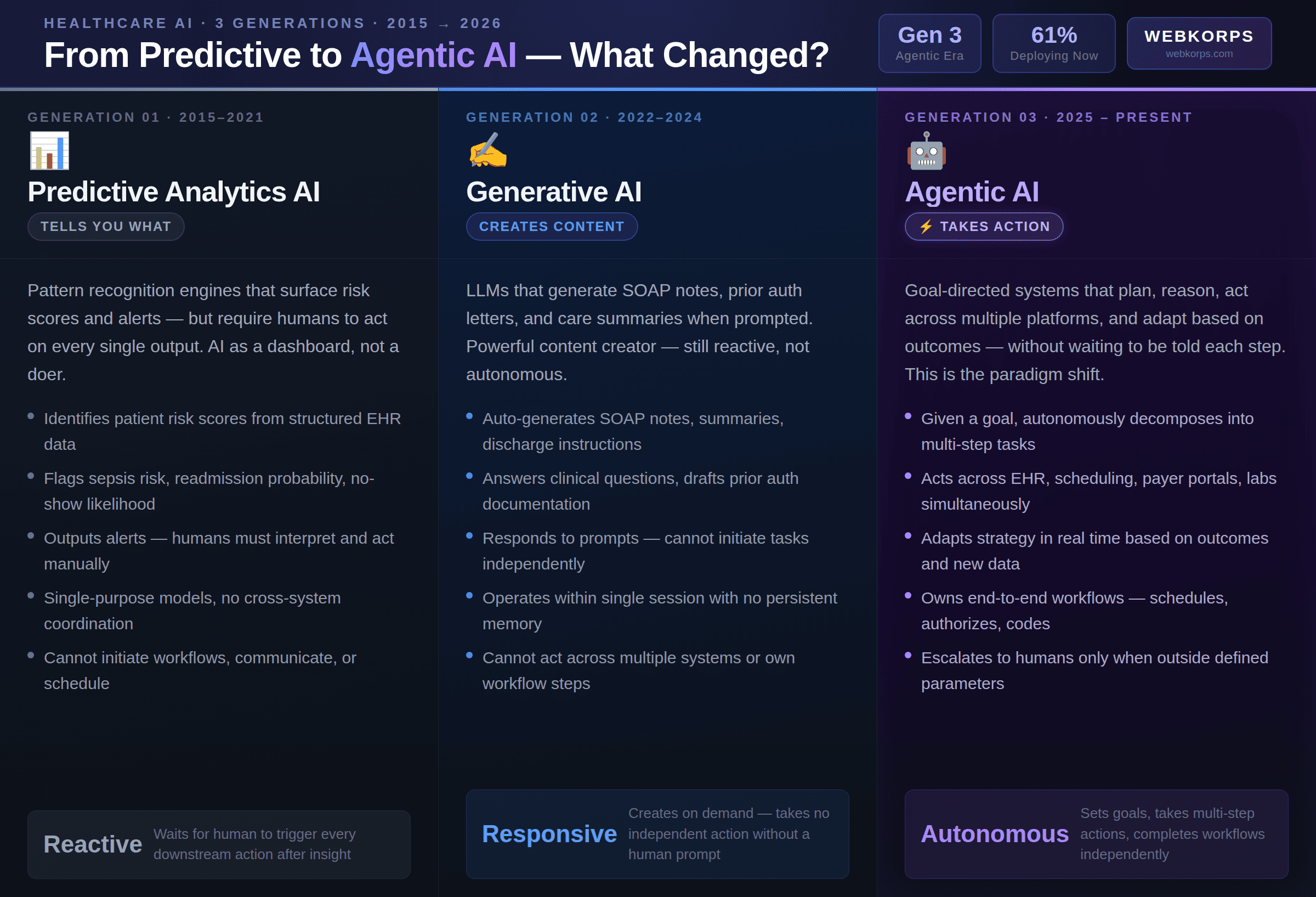
- Generation One – Predictive Analytics (2015–2021): Narrow pattern recognition systems that surface risk scores, clinical alerts, and operational insights – but require a human to act on every output. Generation One AI tells you what is happening; it cannot do anything about it. Sepsis prediction algorithms that flag high-risk patients are classic examples. The AI identifies the pattern; a nurse must read the alert and initiate the intervention.
- Generation Two – Generative AI (2022–2024): Large language models that generate SOAP notes, care summaries, prior authorization letters, and clinical documentation when prompted. Dramatically more capable than prediction-only systems, but still fundamentally reactive. Generative AI creates content on demand – it does not initiate workflows, act across multiple systems, or complete tasks independently without human prompting at each step.
- Generation Three – Agentic AI (2025–Present): Goal-directed autonomous systems that orchestrate end-to-end workflows across multiple platforms – connecting EHRs, scheduling tools, payer portals, laboratory systems, and patient engagement platforms – without waiting to be told each step. Agentic AI does not just answer questions or generate documents. It sets a goal, plans the path, executes the steps, monitors outcomes, and adapts when something changes.
The Four Defining Characteristics of a Healthcare AI Agent
Four specific capabilities separate an authentic AI agent from everything else in the market:
- Goal-directed autonomy: Given an objective (schedule this referral, complete this prior authorization, reconcile these discharge medications), the agent independently determines and executes the required steps without human direction of each action.
- Multi-system action: The agent reaches into EHRs, payer portals, scheduling systems, laboratory systems, and patient communication platforms simultaneously – coordinating across the fragmented ecosystem that makes healthcare administration so expensive.
- Contextual adaptation: The agent changes its approach based on real-time outcomes. If an insurance eligibility check returns a denial, the agent does not stop – it initiates the appeal workflow and alerts the appropriate team member, all without human instruction.
- Bounded human-in-the-loop escalation: Agentic AI is not fully autonomous in a clinical context, nor should it be. Best-practice implementations define explicit escalation paths – the agent handles routine execution autonomously and surfaces specific decisions to human reviewers only when the situation falls outside predefined parameters.
THE CRITICAL DISTINCTION
Generative AI creates content. Agentic AI takes action. This is the operational difference that changes everything in care delivery – and the reason healthcare leaders are moving from pilots to production deployments at an accelerating pace.
What Agentic AI Is NOT
Equally important as understanding what agentic AI is: understanding what it is not, so you can identify vendor hyperbole in the market.
- Not a chatbot: A chatbot answers questions in a conversational interface. An agent initiates multi-step workflows across clinical and administrative systems.
- Not robotic process automation: RPA executes rigid, predefined rule-based scripts. Agents reason about novel situations and adapt their approach based on context and outcomes.
- Not a copilot: A copilot waits for the clinician to ask something. An agent proactively monitors, acts, and escalates without prompting.
- Not a single AI model: The most capable healthcare agentic systems are orchestrated teams of specialized agents – a coordinator agent directing specialist agents for scheduling, documentation, coding, and monitoring, each optimized for its domain.
Also read: Why Agentic AI Makes Current Software Services Obsolete
Anatomy of an AI-Managed Patient Journey – All 7 Stages
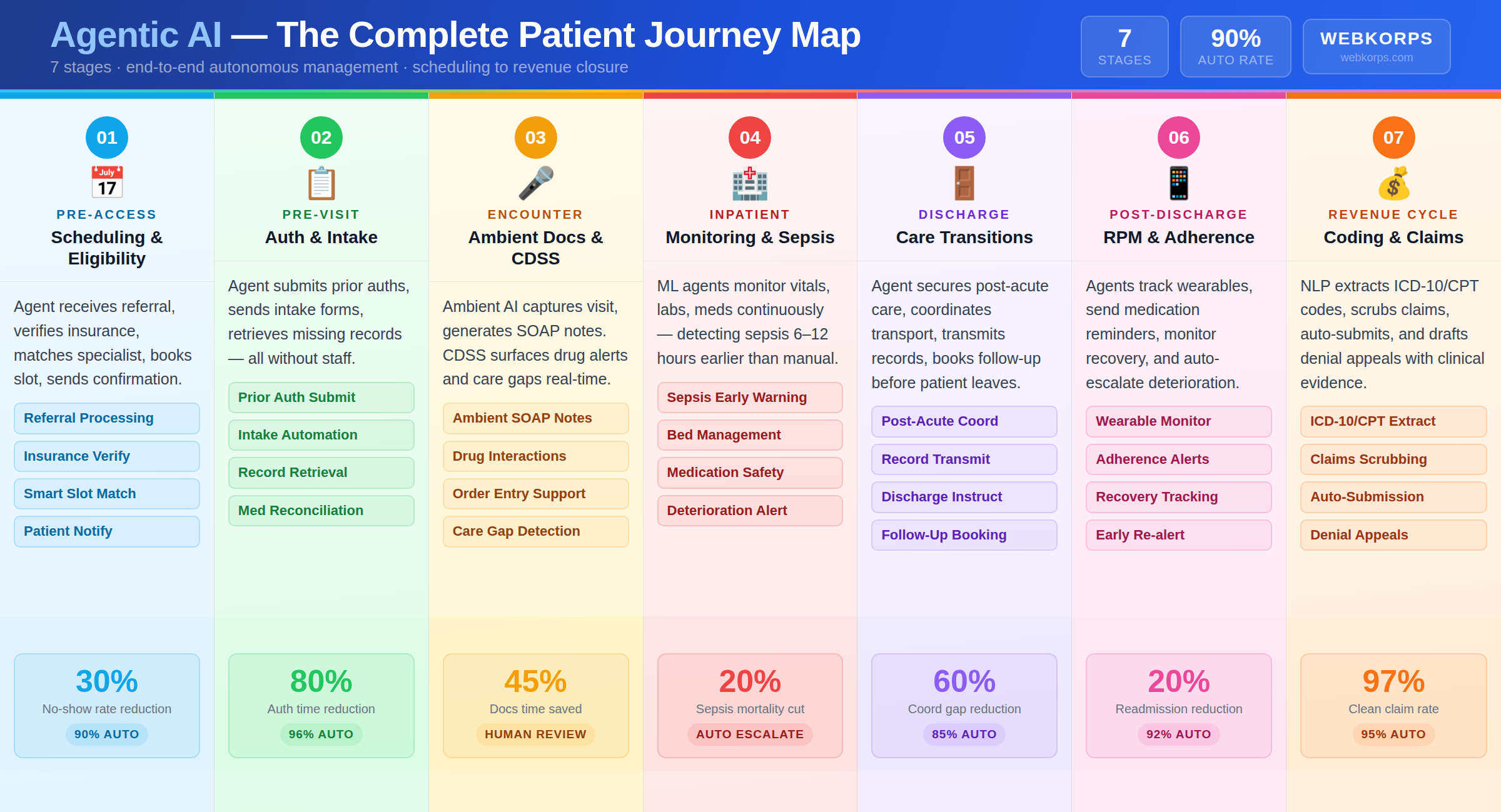
A patient journey contains at least seven distinct stages where coordination failures generate patient harm, care delays, and revenue leakage. Handoff breakdowns between these stages account for a disproportionate share of preventable adverse events and 30-day readmissions. Agentic AI can own or co-own every stage – not as a series of disconnected tools, but as a continuous, goal-directed workflow that follows the patient from referral to revenue closure.
Stage 1: Pre-Access – Autonomous Scheduling and Eligibility Verification
The patient journey begins before the first appointment is booked, and it begins badly for most patients. A referral arrives, sits in a coordinator’s queue, gets processed days later, the patient is reached by phone on the third attempt, scheduling takes 12 minutes, and nobody verifies insurance eligibility until the patient shows up for the appointment.
An agentic AI scheduler receives the referral trigger, immediately queries the payer database for real-time eligibility, matches the patient to the most appropriate specialist based on condition severity, network status, and provider availability, books the optimal appointment slot, sends a confirmation to the patient, and routes intake forms tailored to the specific condition – all autonomously, in minutes. UnityAI’s scheduling agents complete 90 percent of these tasks fully autonomously, requiring human escalation less than 6 percent of the time, delivering a 26 percent improvement in scheduler productivity and a 30 percent reduction in no-show rates in production.
Stage 2: Pre-Visit – Prior Authorization, Intake, and Record Retrieval
Prior authorization is among the most despised administrative processes in healthcare – time-consuming, often arbitrary, and deeply damaging to care continuity. A 2024 survey found that 99 percent of clinicians and 96 percent of office administrators are comfortable with AI assisting in prior authorization decisions when appropriate safeguards are in place.
An agentic prior authorization workflow: the agent pulls the procedure code and diagnosis from the EHR, queries the payer portal for authorization requirements, generates the clinical justification documentation using the patient’s record, submits the request, monitors status, and – if denied – autonomously drafts an appeal with supporting clinical evidence. The same agent simultaneously requests missing records from referring physicians and sends personalized intake forms to the patient, pre-populated where data is already available. What previously took 11 days of phone calls and manual documentation now completes in under 2 hours.
Stage 3: Clinical Encounter – Ambient Documentation and CDSS Support
During the clinical encounter, two categories of agentic AI deliver the most immediate value to the physician. First, ambient documentation agents passively capture the physician-patient conversation and generate structured SOAP notes, HPI summaries, and billing-ready encounter documentation without the physician typing a single character. Multiple health systems have documented 45 to 50 percent reductions in documentation time following ambient AI deployment. Clinicians describe getting their evenings back.
Second, clinical decision support agents running in the background surface real-time alerts: drug-drug interactions that the human prescriber may not have recognized across a complex medication list, care gap warnings for screenings the patient is overdue for, evidence-based differential diagnosis suggestions when the clinical picture is ambiguous, and appropriate order sets based on the working diagnosis. Critical distinction: in Stage 3, agentic AI supports and augments clinical decision-making. The physician retains full decision authority. Agents that cross the line into autonomous clinical decision-making without physician oversight represent both a regulatory risk and a patient safety concern.
Stage 4: Inpatient Monitoring – Continuous Surveillance and Sepsis Detection
For admitted patients, agentic AI agents continuously monitor the full data stream – vital signs, laboratory values, medication administrations, nursing notes, fluid balances – applying machine learning models that identify deterioration patterns invisible to human reviewers managing dozens of simultaneous patients. The clinical impact is significant: ML-based sepsis detection agents identify sepsis 6 to 12 hours before standard clinical criteria are triggered, enabling early antibiotic administration that reduces mortality by up to 20 percent. Bed management agents coordinate real-time capacity planning, discharge readiness assessments, and post-acute bed availability – reducing boarding time and improving patient flow. Medication safety agents verify dosing against the complete patient profile at every administration event.
Stage 5: Discharge – Care Transition Coordination
Discharge is the highest-risk transition in the patient journey. Studies consistently show that the 30-day readmission risk is highest in the first 72 hours post-discharge, when the coordination gap between inpatient and outpatient care is widest. The critical interventions – follow-up appointment booked before leaving, post-acute bed secured, complete medication reconciliation performed, discharge instructions delivered at an appropriate literacy level, and records transmitted to the receiving facility – happen inconsistently because human care coordinators managing high census simply cannot execute all of them reliably for every patient.
An agentic discharge coordination agent owns all of these steps simultaneously. Before the discharge order is signed, the agent has checked post-acute bed availability, coordinated transport, transmitted the complete discharge summary to the receiving facility, reconciled inpatient and outpatient medications for discrepancies, booked the follow-up appointment, and sent condition-specific, literacy-appropriate discharge instructions to the patient’s preferred communication channel. The agent does not wait to be asked. It anticipates and acts.
Stage 6: Post-Discharge – Remote Monitoring and Adherence Management
The first 30 days after discharge represent the highest-risk period for readmission, medication errors, and care plan deviation. Agentic AI extends the care team’s reach into this critical window at a scale no human workforce can match. Remote patient monitoring agents continuously process data from wearable devices, home blood pressure cuffs, and continuous glucose monitors – applying predictive models to identify early warning signals of deterioration before they become acute events. Medication adherence agents send personalized reminders calibrated to the patient’s communication preferences, monitor adherence patterns, and escalate missed doses or concerning trends to the care team for intervention. The combination of proactive monitoring and intelligent escalation has produced 20 percent reductions in 30-day readmission rates in documented deployments.
Stage 7: Revenue Cycle Closure – Coding, Claims, and Denial Management
The final stage of the patient journey is invisible to the patient but critical to the health system’s financial sustainability. Manual medical coding – the process of translating clinical documentation into ICD-10 diagnoses and CPT procedure codes – achieves industry-average clean claim rates of approximately 82 percent. The remaining 18 percent of claims are returned with errors, generating denial management workloads that cost the system more to process than the claims are worth.
Agentic coding agents apply NLP to extract diagnoses, procedures, and supporting documentation from clinical notes in real time, assign appropriate ICD-10 and CPT codes, scrub the claim for accuracy and compliance before submission, and flag any documentation gaps that could trigger denials. Documented outcomes include clean claim rates of 97 percent or higher, 25 percent faster reimbursement cycles, and 60 percent reductions in coding labor. When denials do occur, denial management agents autonomously generate appeals with supporting clinical evidence drawn from the patient record – without any human involvement until the appeal is ready for review.
Real-World Deployments – Who Is Already Doing This at Scale?
Agentic AI in healthcare is no longer a research concept or a vendor pitch deck promise. The following represent verified, production-scale deployments that have moved beyond pilot programs:
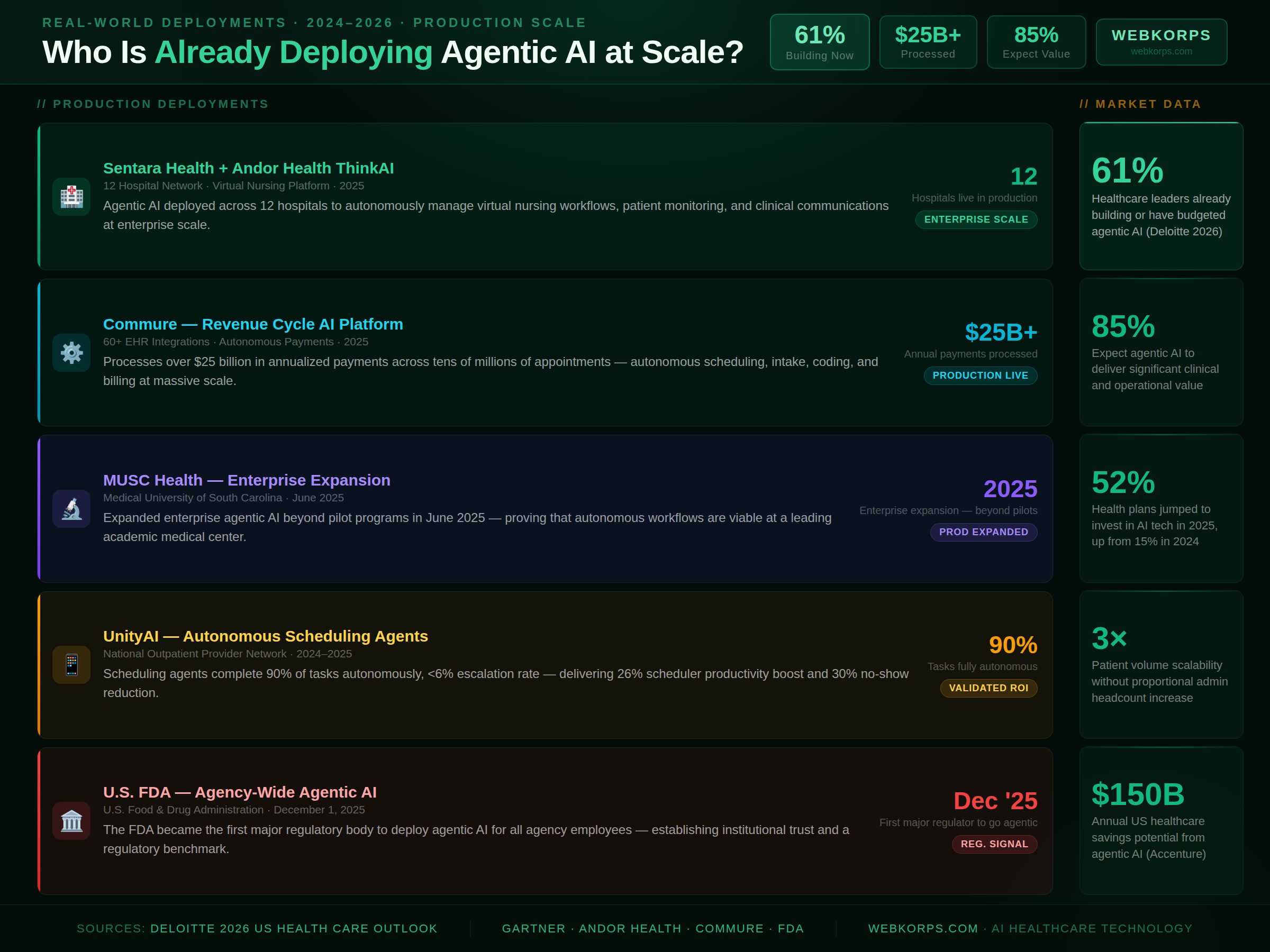
Sentara Health and Andor Health ThinkAI – 12-Hospital Virtual Nursing Platform
Sentara Health, one of the largest nonprofit integrated health systems in the US, partnered with Andor Health to deploy ThinkAI, an agentic AI virtual nursing platform, across 12 hospitals. The platform autonomously manages nursing workflow prioritization, patient monitoring alerts, care team communications, and clinical documentation at enterprise scale – demonstrating that agentic nursing workflows are viable in complex, high-acuity environments.
Commure – Revenue Cycle at $25 Billion in Annualized Payments
Commure’s agentic AI platform now serves tens of millions of appointments, processes more than $25 billion in annualized payments, and integrates with over 60 EHR systems. The platform deploys autonomous agents for patient access, intake, scheduling, clinical documentation, and medical coding – representing the most at-scale deployment of agentic AI across the complete revenue cycle in the industry.
MUSC Health – Enterprise Agentic AI Expansion
The Medical University of South Carolina expanded enterprise agentic AI deployments in June 2025, moving beyond pilot programs to systematic autonomous workflow deployment across clinical and administrative functions. MUSC Health’s expansion is significant because it demonstrates that leading academic medical centers – traditionally cautious adopters – are now committing to production agentic AI infrastructure.
UnityAI Scheduling Agents – Validated ROI at Scale
UnityAI’s autonomous scheduling agent platform achieved a 90 percent autonomous task completion rate with less than 6 percent human escalation – delivering a 26 percent improvement in scheduler productivity and a 30 percent reduction in no-show rates for a national outpatient provider network. These are not projected outcomes from a modeling exercise. They are validated results from a production system processing millions of patient interactions.
The FDA – First Major Regulatory Body to Go Fully Agentic
On December 1, 2025, the U.S. Food and Drug Administration became the first major regulatory body to deploy agentic AI for all agency employees. The FDA’s adoption of autonomous AI workflows for administrative and analytical functions represents a significant institutional trust signal – and sets the benchmark for responsible agentic AI deployment in regulated healthcare environments.
| Organization | Application | Key Outcome | Scale |
| Sentara Health + Andor Health | Virtual nursing + monitoring | Enterprise-scale autonomous nursing | 12 hospitals |
| Commure | Full revenue cycle | $25B+ annual payments processed | 60+ EHR integrations |
| MUSC Health | Enterprise AI expansion | Beyond pilot to production | Academic medical center |
| UnityAI | Autonomous scheduling | 30% no-show reduction | National network |
| U.S. FDA | Agency-wide agentic AI | First major regulator to adopt | All employees |
The Benefits – Why Healthcare Leaders Are Moving Fast
The case for agentic AI in healthcare is not built on theoretical projections. It is built on documented, production-validated outcomes across multiple health systems and use cases. Here are the six most significant benefit categories with specific performance data:
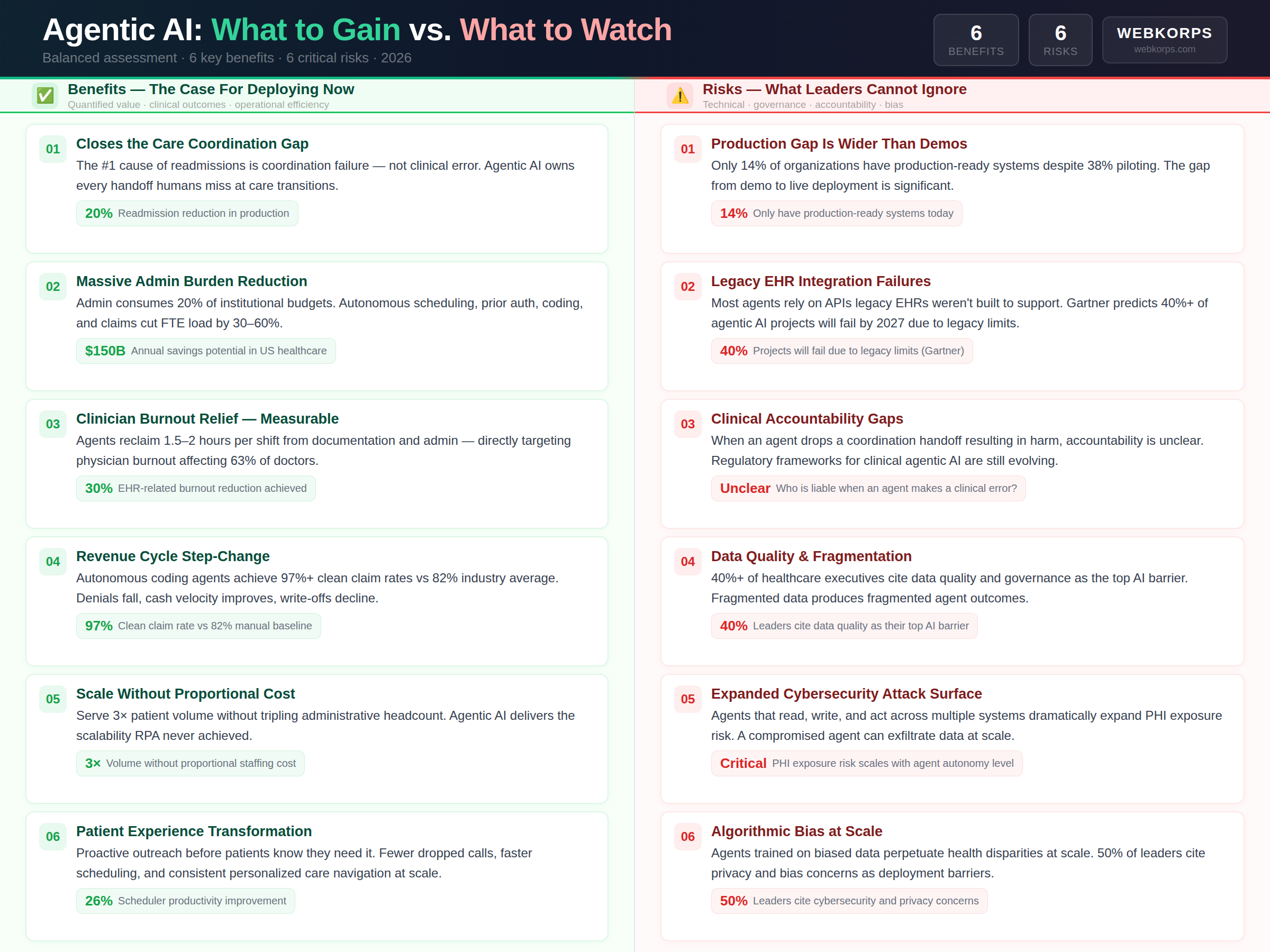
1. Closing the Care Coordination Gap – The Root Cause of Readmissions
The most preventable driver of hospital readmissions and post-discharge adverse events is not clinical failure – it is coordination failure. A follow-up appointment was not booked. A medication reconciliation was not completed. A post-acute bed was not confirmed before discharge. A specialist note was not transmitted to the primary care provider. Each of these failures is banal in isolation and catastrophic in aggregate.
Agentic AI addresses care coordination failures at the structural level by owning the handoffs that fall through human systems. When an agent is responsible for the complete transition workflow – not a single step in it – the handoffs do not get dropped because the agent does not forget, get overwhelmed by census, or end their shift. Documented outcome: 20 percent reduction in 30-day readmissions in production deployments with agentic post-discharge management.
2. Administrative Burden Reduction – Attacking the 20% Budget Drain
Administrative tasks consume approximately 20 percent of total healthcare institutional budgets in the United States – an estimated $1 trillion annually in a $5 trillion healthcare system. A significant portion of this cost is structurally reducible through autonomous agent workflows. Scheduling, insurance eligibility verification, prior authorization, medical coding, claims submission, and denial management are all high-volume, rules-based processes that agentic AI can execute with higher accuracy and dramatically lower unit cost than manual labor. Documented reductions in manual FTE load across these functions range from 30 to 60 percent in production implementations, with full payback periods typically under 18 months.
3. Clinician Burnout Relief – Getting Physicians Their Time Back
Physician burnout is a population-level crisis in American medicine. Sixty-three percent of physicians identify EHR documentation as their primary burnout driver. The average physician spends 4.5 hours per day on EHR-related tasks – more time than they spend in direct patient care. Agentic AI, specifically ambient documentation agents, directly attacks this problem by eliminating the majority of the transcription and documentation burden. Combined with autonomous prior authorization handling, the documented impact is 1.5 to 2 hours reclaimed per clinical shift – returned to direct patient care and physician well-being.
4. Revenue Cycle Performance – From 82% to 97% Clean Claim Rate
The financial performance difference between 82 percent and 97 percent clean claim rates is not marginal. For a health system processing $500 million in annual claims, improving clean claim rates from 82 to 97 percent eliminates approximately $75 million in denial management costs, rework labor, and write-offs annually. Agentic coding and claims management agents achieve these outcomes by eliminating the human error, workload bottlenecks, and knowledge gaps that make manual coding inherently imprecise. The improvement is not incremental – it is a structural performance step-change.
5. Patient Experience Transformation – Proactive, Not Reactive
From the patient’s perspective, an agentic AI-managed care journey looks radically different from the conventional experience. Instead of missing a follow-up appointment because no one called, the patient receives a confirmation before leaving the hospital. Instead of waiting 11 days for prior authorization, the request is submitted and approved (or appealed) automatically. Instead of being surprised by a readmission because no one noticed the worsening symptoms, the remote monitoring agent has already escalated to the care team. Agentic AI enables health systems to shift from reactive care delivery to proactive patient engagement at scale – a transformation that no staffing increase could achieve at equivalent cost.
6. Scalability Without Proportional Cost Growth
This is perhaps the most strategically significant benefit for health system leaders facing population growth, aging demographics, and workforce shortages simultaneously. Agentic AI delivers scalability that traditional staffing models cannot. A health system can double its patient volume served through autonomous scheduling, prior authorization, and care coordination without doubling its administrative headcount. The marginal cost of an additional agentic AI workflow task is near zero once the infrastructure is deployed – a fundamentally different cost structure from any labor-intensive administrative model.
Also read: Cost to Build an AI-Powered Healthcare App
The Risks – What Healthcare Leaders Cannot Afford to Ignore
A responsible assessment of agentic AI in healthcare requires acknowledging significant risks alongside the benefits. Healthcare leaders who deploy agentic AI without rigorous risk management will face outcomes ranging from technical failure to patient harm to regulatory action. The following six risks demand explicit planning before any production deployment:
1. The Production Gap Is Wider Than Vendor Pitches Suggest
Industry data reveals a stark reality: while 30 percent of organizations are exploring agentic AI and 38 percent are piloting solutions, only 14 percent have production-ready agentic systems. The gap between a compelling demo and a system that performs reliably in a complex, high-stakes clinical environment is significant. Healthcare technology procurement teams need to insist on production performance evidence from comparable deployments – not demo environments, not projected outcomes, and not single-metric pilot results. Gartner’s research indicates that over 40 percent of agentic AI projects will fail by 2027, primarily because organizations underestimate the complexity of real-world production deployment.
2. Legacy EHR Integration Failures
The majority of US health systems operate on an EHR infrastructure that was not designed to support the event-driven, real-time API access patterns that agentic AI requires. Epic, Cerner, and MEDITECH have made significant progress with FHIR R4 APIs – but many legacy modules and third-party systems still rely on batch processing, HL7 v2 message queues, or proprietary interfaces that create bottlenecks and limit agent capabilities. Gartner explicitly predicts that legacy system incompatibility will be the primary cause of agentic AI project failures through 2027. Before committing to an agentic AI implementation, health system CIOs must conduct a thorough integration readiness assessment of their complete EHR ecosystem.
3. Clinical Accountability Gaps – Who Is Responsible When an Agent Fails?
This is the question that keeps healthcare legal and compliance teams awake at night, and appropriately so. When an autonomous agent drops a care coordination handoff, fails to escalate a deteriorating patient signal, or generates an incorrect prior authorization – resulting in delayed care – the accountability chain is not clearly established in current regulatory frameworks. Is the physician liable? The health system? The AI vendor? The engineer who designed the escalation thresholds? Regulatory guidance is evolving, but organizations deploying agentic AI today must establish explicit accountability frameworks, document agent boundaries and escalation criteria, and ensure their malpractice coverage addresses AI-assisted care scenarios.
4. Data Quality and Fragmentation
Agentic AI is only as good as the data it acts on. In healthcare environments where patient data is fragmented across multiple EHRs, disconnected departmental systems, and incomplete historical records, agent performance will be directly limited by data quality. Over 40 percent of healthcare executives identify data quality, standardization, and governance as their primary barrier to AI implementation. Before deploying agentic workflows, organizations need a unified patient data strategy – ideally built on a FHIR-native data platform – that provides agents with complete, current, and reliable information to act on.
5. Expanded Cybersecurity Attack Surface
Autonomous agents that can authenticate across multiple healthcare systems, read PHI, write clinical documentation, and initiate financial transactions represent a dramatically expanded cybersecurity attack surface compared to traditional single-purpose software. A compromised agentic AI system does not just expose data – it can actively execute harmful workflows at scale across every system the agent can access. Healthcare organizations must apply zero-trust security architecture to all agentic AI deployments, with strict scope limitation, comprehensive audit logging of every agent action, anomaly detection for agent behavior, and explicit PHI access minimization built into the agent design.
6. Algorithmic Bias and Health Equity Risks
AI systems trained on historical healthcare data will encode the biases present in that data – and in healthcare, those biases have well-documented disparate impacts on Black, Hispanic, and low-income patient populations. When agentic AI systems automate risk stratification, resource allocation, and care prioritization at scale, biased algorithms do not just affect individual patients – they systematically perpetuate health disparities across entire populations. Organizations deploying agentic AI must conduct bias audits on every clinical model before production deployment, implement ongoing bias monitoring, and establish equity metrics as first-class performance indicators alongside clinical and financial outcomes.
Governance Framework for Responsible Autonomous Healthcare AI
The organizations that will derive the most sustained value from agentic AI are not those that deploy it fastest – they are those that deploy it most thoughtfully, with governance frameworks that enable confident expansion over time. The following framework represents best practices drawn from the most successful enterprise healthcare AI deployments in 2025 and 2026.
The Bounded Autonomy Model
The most durable governance approach for clinical agentic AI is the bounded autonomy model: clearly defined tiers of agent authority, with explicit escalation protocols for each tier. Most organizations will deploy agentic AI with layered checkpoints and human oversight structures that balance efficiency with control. The tiering typically looks like this:
| Autonomy Tier | Actions Included | Human Role | Examples |
| Fully Autonomous | Routine, reversible, low-risk | Monitoring and audit only | Appointment reminders, eligibility checks, claim submissions |
| Human-Reviewed | High-value, consequential | Review before action | Prior auth decisions, discharge planning, escalation routing |
| Human-Decided | Clinical judgment required | Full decision authority | Treatment decisions, high-risk patient alerts, protocol deviations |
Explainability and Audit Requirements
Every agentic AI action in a healthcare context must be logged, attributable, and explainable. Regulators, clinicians, malpractice attorneys, and patients will all ask ‘why did the AI do that?’ – and the system must be architecturally capable of answering that question with specificity. This means maintaining immutable audit logs of every agent action, preserving the reasoning chain that led to each action, and building explainability into the agent design from the first line of architecture – not as an afterthought.
HIPAA, HITECH, and the Evolving Agentic AI Regulatory Landscape
Agentic AI systems that access, act on, and transmit Protected Health Information must operate within HIPAA-compliant infrastructure under HITECH security requirements. Every vendor, tool, and service in the agent’s tool chain must execute a Business Associate Agreement. Organizations also need to monitor emerging AI-specific regulations: the FDA is developing Software as a Medical Device (SaMD) guidance that will directly affect clinical agentic AI, and the CMS has issued preliminary guidance on AI-assisted prior authorization that is likely to evolve significantly through 2026 and 2027. The FDA’s December 2025 institutional adoption of agentic AI for all agency employees signals that the regulatory body is developing deep operational familiarity with the technology – a harbinger of more specific guidance to come.
Continuous Monitoring and Drift Detection
Production agentic AI systems are not static deployments. Model performance drifts as clinical practice evolves, patient population demographics shift, and payer policies change. Organizations must implement continuous performance monitoring that tracks task completion rates, escalation rates, outcome metrics, and bias indicators on an ongoing basis – not just at deployment. Scheduled model revalidation, real-world performance benchmarking against clinical outcomes, and rapid response protocols for detected drift are all essential components of mature agentic AI governance.
Also read: HIPAA-Compliant AI Software Development
How to Build an Agentic AI Patient Journey Platform – Practical Roadmap
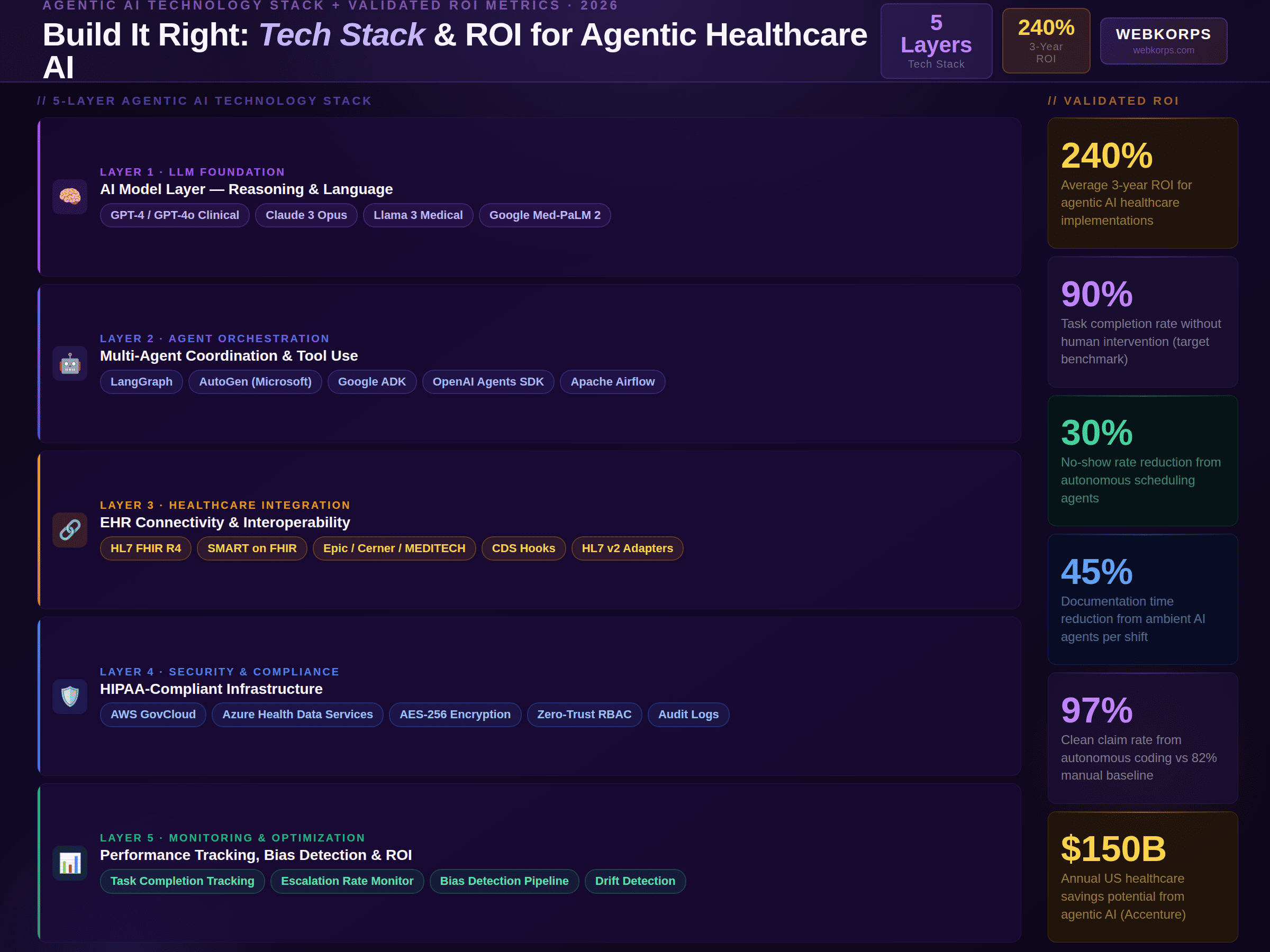
The Four Infrastructure Prerequisites
Before deploying any agentic AI workflow, four infrastructure prerequisites must be in place. Attempting to deploy agents without these foundations is the most common cause of project failure:
- Bi-directional EHR integration with event-driven triggers: Agents need real-time access to clinical events as they happen – not batch-processed data from the previous night. This requires FHIR R4 subscription APIs or equivalent event streams from every connected system.
- Unified patient data platform: Agents operating on fragmented data will produce fragmented outcomes. A consolidated patient data layer – ideally built on a FHIR-native platform with standardized terminology mapping – gives agents the complete, reliable information they need to act correctly.
- Workflow orchestration layer: A multi-agent system needs an orchestration layer that routes tasks between specialized agents, manages state across long-running workflows, handles failures gracefully, and maintains the audit trail of all agent actions.
- HIPAA-compliant cloud infrastructure: AWS GovCloud, Azure Health Data Services, or Google Cloud Healthcare API – all provide HIPAA BAAs, compliant configurations, and the healthcare-specific API capabilities that agentic workloads require.
Recommended First Deployment: High-Value, Low-Risk Use Cases
The most successful agentic AI healthcare implementations start with a narrow, well-defined use case that delivers rapid, measurable ROI and builds organizational confidence before expanding scope. The following four use cases represent the optimal starting points based on documented deployment outcomes:
- Autonomous appointment scheduling and no-show management: High volume, low clinical risk, immediate measurable outcome (no-show rates, scheduler productivity). Ideal first deployment.
- Insurance eligibility verification and prior authorization: Clear success metrics (approval time, denial rate), high administrative ROI, and clinician satisfaction improvement are measurable.
- Post-discharge follow-up outreach and remote monitoring: Direct link to 30-day readmission rate – a metric every health system CEO monitors. Clean causal chain from agent deployment to outcome improvement.
- Autonomous medical coding from clinical documentation: Clean claim rate is an immediately measurable financial outcome. Revenue cycle teams will see the impact within the first billing cycle after deployment.
The Multi-Agent Architecture for Healthcare
The most capable healthcare AI systems are not single, all-powerful models. They are orchestrated teams of specialized agents, each optimized for its specific domain, coordinated by an orchestrator that manages state, routes tasks, and handles failures. A typical multi-agent patient journey architecture includes:
- Coordinator Agent: Receives high-level objectives (complete discharge coordination for patient X), decomposes them into tasks, and routes them to specialist agents.
- Scheduling Specialist Agent: Manages all appointment booking, rescheduling, eligibility verification, and no-show prediction.
- Authorization Specialist Agent: Handles prior authorization submission, status monitoring, denial detection, and appeal generation.
- Documentation Specialist Agent: Ambient capture, SOAP note generation, coding, and clinical summary creation.
- Monitoring Specialist Agent: Continuous vital sign and RPM data processing, deterioration detection, and care team escalation.
- Revenue Cycle Specialist Agent: Claims generation, scrubbing, submission, status tracking, and denial management.
Measuring Agentic AI ROI – Key Performance Indicators
Define these metrics before deployment and measure them continuously. ROI that cannot be measured cannot be defended at the next board meeting:
| KPI | Baseline (Manual) | AI Target | Business Impact |
| Task completion rate (no human) | 0% | >85% | Administrative FTE reduction |
| Scheduling no-show rate | ~22% industry avg | <15% | Revenue recovery + capacity |
| Prior auth approval time | 11 days average | <2 hours | Care delay elimination |
| Clean claim rate | 82% industry avg | >97% | $M in denial reduction |
| Documentation time per encounter | 16 min avg | <8 min | Burnout reduction + capacity |
| 30-day readmission rate | Baseline varies | -20% | Quality metrics + penalties |
| Coding accuracy rate | ~88% | >96% | Revenue integrity |
The Future – Where Agentic Patient Journey Management Is Heading
Multi-Agent Ecosystems Across the Full Care Continuum by 2028
By 2028, leading health systems will operate fleets of hundreds of coordinated, specialized AI agents – each governed, each monitored, each contributing to a patient journey that no human coordination team could manage at equivalent scale, consistency, or cost. The trajectory is not speculative: it is the direct extrapolation of current deployment rates, infrastructure investment, and capability advancement in foundation models and agent orchestration frameworks.
Proactive Population Health Management at Agent Scale
The most strategically significant long-term application of agentic AI is not in reactive care delivery – it is in proactive population health management. Agents that continuously monitor attributed patient populations, identify individuals with early-stage deterioration signals or care gaps, initiate outreach before acute events occur, and coordinate preventive interventions autonomously represent the shift from sick care to health care that every healthcare system claims as a strategic goal but few have the operational infrastructure to deliver. Agentic AI provides that infrastructure.
Payer-Provider Agent Coordination – Eliminating the Administrative Layer
The most expensive friction in the US healthcare system is the administrative layer between payers and providers – prior authorization, claims adjudication, coverage disputes, and care plan coordination. Autonomous agents on both sides of the payer-provider relationship are beginning to negotiate, coordinate, and resolve these processes in real time, eliminating the fax-and-phone infrastructure that currently consumes hundreds of billions of dollars annually in administrative waste. Commure’s $25 billion in annualized autonomous payment processing is an early indicator of what this coordination capability will look like at full deployment scale.
The Hybrid Workforce – Agents Augment, Not Replace
Nearly half of healthcare leaders anticipate deeper human-AI collaboration within the next three to five years – reinforcing the consensus view that the optimal healthcare delivery model is not one where agents replace clinical and operational staff, but one where agents handle the routine, rules-based, high-volume work that currently prevents skilled humans from focusing on the judgment-intensive tasks that genuinely require human expertise. Radiologists who review AI-triaged imaging rather than spending half their day on normal studies. Nurses whose cognitive load is reduced by continuous monitoring agents rather than expanding because of census growth. Physicians who spend their time thinking about complex patients rather than typing clinical notes. This is the hybrid workforce model that the most thoughtful health system leaders are building toward.
Why Webkorps for Agentic AI Healthcare Development
Building a production-grade agentic AI patient journey platform is not a technology project – it is a systems integration, clinical workflow, regulatory compliance, and data architecture project that happens to involve cutting-edge AI. The organizations that succeed are those that partner with development teams who understand all of these dimensions simultaneously.
Webkorps brings an end-to-end agentic AI development capability specifically built for healthcare. Our teams have deep expertise in EHR integration across Epic, Cerner, MEDITECH, and athenahealth – including the complex FHIR R4 subscription API and HL7 v2 adapter configurations that agentic workflows require. We build HIPAA compliance into the architecture from the first design decision, not as a post-hoc retrofit. Our multi-agent system design and orchestration capability spans the complete technology stack – from LLM selection and clinical fine-tuning through agent framework implementation, EHR integration, security hardening, and production deployment.
We have worked with healthcare organizations across the full spectrum – from regional health systems deploying their first autonomous scheduling workflow to enterprise health networks building comprehensive multi-agent patient journey platforms. Our delivery approach is grounded in the reality that the gap between a compelling agentic AI demo and a production system that performs reliably in a complex clinical environment is significant – and navigating that gap requires experience, not just capability.
| Webkorps Capability | Description |
| End-to-End Agentic AI Development | From architecture design through production deployment and ongoing optimization |
| EHR Integration Expertise | Epic, Cerner, MEDITECH, athenahealth – FHIR R4, SMART on FHIR, HL7 v2 |
| HIPAA-Compliant Engineering | Security and compliance built in from day one, not added as an afterthought |
| Multi-Agent System Design | Coordinator + specialist agent architecture, orchestration, and state management |
| Clinical AI Fine-Tuning | Domain-specific model adaptation for clinical documentation, coding, and CDSS |
| Production Monitoring | Drift detection, bias monitoring, performance dashboards, and ongoing optimization |
| READY TO BUILD? |
| Schedule a discovery call with Webkorps to assess your agentic AI readiness, define your first deployment use case, and design the architecture that will scale with your organization. Visit webkorps.com or contact our healthcare AI team directly. |
The Window to Lead Is Open – But Not Indefinitely
The transformation of healthcare delivery through agentic AI is not a question of whether it will happen. It is already happening. Sentara Health, MUSC Health, Commure, and the US FDA have all crossed from exploration to production deployment. Sixty-one percent of healthcare leaders have committed budget. Eighty-five percent expect significant value. The infrastructure is maturing, the models are improving, and the governance frameworks are crystallizing.
The question for healthcare leaders reading this in 2026 is not ‘should we invest in agentic AI?’ The question is ‘how do we deploy it responsibly, rapidly, and in a way that builds toward a comprehensive capability rather than a collection of disconnected pilots?’
The answers require getting four things right simultaneously: the technical architecture (multi-agent, FHIR-native, HIPAA-compliant by design); the governance framework (bounded autonomy, explicit escalation, continuous monitoring); the integration strategy (starting with high-value, low-risk use cases that generate early ROI); and the right development partner (one who understands healthcare workflows, EHR integration complexity, and regulatory requirements as deeply as they understand the AI technology itself).
Organizations that get these four things right in 2026 will be operating autonomous patient journey platforms by 2027 – delivering better patient outcomes, lower administrative costs, reduced clinician burnout, and stronger financial performance than their peers. The competitive moat that comes from 12 months of production agentic AI experience will be difficult to close.
Organizations that wait will spend 2027 and 2028 catching up.
TAKE THE NEXT STEP WITH WEBKORPS
Webkorps specializes in building production-grade agentic AI healthcare platforms – from architecture design through deployment and beyond. Our healthcare AI team is ready to help you assess your readiness, define your first deployment, and build the platform that will transform your patient journey. Contact us at webkorps.com to schedule your discovery session.
Frequently Asked Questions: Agentic AI in Healthcare
What is agentic AI in healthcare?
Agentic AI in healthcare refers to autonomous AI systems capable of planning, reasoning, and executing multi-step workflows across clinical and administrative platforms – without requiring human instruction at each step. Unlike predictive AI (which identifies risks) or generative AI (which creates content when prompted), agentic AI takes independent action: scheduling appointments, submitting prior authorizations, generating clinical documentation, monitoring patients, and managing revenue cycle processes – all based on defined goals and bounded authority parameters set by the health system.
How does agentic AI differ from generative AI in clinical settings?
Generative AI in healthcare creates content when prompted – SOAP notes, discharge summaries, prior auth letters – but waits for human instruction at every step. Agentic AI takes autonomous action: given a goal (complete this patient’s discharge coordination), it independently executes all required tasks across multiple systems, adapts to obstacles, and escalates only when the situation exceeds its defined authority parameters. The distinction is reactive versus proactive, single-step versus multi-step, and content creation versus workflow execution.
Can agentic AI make clinical decisions autonomously?
Best-practice agentic AI implementations use a bounded autonomy model in which clinical decision authority remains with the physician. Agents handle administrative and coordination tasks fully autonomously – scheduling, prior authorization, documentation, coding – and support clinical decision-making by surfacing alerts, evidence, and recommendations. Final clinical decisions involving treatment selection, medication changes, and care plan modifications require physician authorization. This is not a technical limitation – it is a deliberate governance design choice that reflects appropriate patient safety and liability management.
What patient journey stages can AI agents manage today?
As of 2026, production-validated agentic AI deployments are managing all seven major patient journey stages: pre-access scheduling and eligibility verification, pre-visit prior authorization and intake, clinical encounter documentation and CDSS support, inpatient monitoring and sepsis detection, discharge care coordination, post-discharge remote monitoring and adherence management, and revenue cycle coding, claims, and denial management. The most advanced deployments coordinate all seven stages through a unified multi-agent architecture.
What are the biggest risks of deploying agentic AI in hospitals?
The six primary risks requiring proactive management are:
- The production gap between demos and live clinical performance.
- legacy EHR integration failures that limit agent capabilities.
- unclear clinical accountability when agents fail.
- data quality and fragmentation issues that degrade agent performance.
- expanded cybersecurity attack surface from multi-system agent access.
- algorithmic bias that can perpetuate health disparities at scale.
Organizations that deploy with explicit governance frameworks addressing all six risks achieve significantly better outcomes than those that treat these as secondary concerns.
Is agentic AI HIPAA compliant?
Agentic AI can be fully HIPAA-compliant when implemented correctly. Compliance requires: deployment on HIPAA-compliant cloud infrastructure (AWS GovCloud, Azure Health Data Services, or Google Cloud Healthcare API); Business Associate Agreements with every vendor in the agent’s tool chain; AES-256 encryption of all PHI at rest and in transit; role-based access control limiting agent PHI access to the minimum necessary for each task; immutable tamper-proof audit logs of every agent action; and de-identification of any data used for agent model training. HIPAA compliance is an architecture decision, not a compliance checkbox – it must be built in from the first design conversation.
What does it cost to build an agentic AI patient journey platform?
Development investment for a production agentic AI patient journey platform varies significantly based on scope, EHR complexity, and starting infrastructure maturity. A focused first deployment – autonomous scheduling with eligibility verification and no-show management – can be production-ready in 12 to 16 weeks at a fraction of the cost of a full-platform build. A comprehensive multi-agent platform spanning all seven patient journey stages typically requires 9 to 18 months of development. In both cases, documented ROI timelines in comparable deployments run 12 to 18 months to full payback, with a 3-year ROI of 200 to 240 percent. Webkorps recommends a phased deployment approach that generates measurable ROI from each phase while building toward the comprehensive platform.
Which health systems are already using agentic AI at scale?
Confirmed production-scale deployments as of 2026 include: Sentara Health deploying ThinkAI virtual nursing agents across 12 hospitals; Commure processing over $25 billion in annualized payments through autonomous revenue cycle agents across 60+ EHR integrations; MUSC Health expanding enterprise agentic AI beyond pilot programs; UnityAI delivering 90 percent autonomous scheduling completion rates for a national outpatient provider network; and the US FDA deploying agentic AI for all agency employees. Beyond these public examples, multiple large integrated delivery networks are in production or late-stage deployment – the rate of enterprise adoption accelerated significantly in 2025 and continues to accelerate in 2026.

