Table of Contents
Key Takeaways
Healthcare AI has moved beyond pilot programs to deliver measurable financial returns, with 85% of executives reporting increased revenue and 80% seeing reduced costs in 2026.
- AI-powered clinical documentation saves physicians 2-30 minutes per appointment and generates $300,000 annually per physician through ambient listening technology that automates note-taking during patient visits.
- Automated medical coding and billing systems deliver 20-72% productivity increases and ROI within 1-3 months by reducing manual errors that cost the healthcare system $36 billion yearly.
- Prior authorization automation achieves 5x ROI and processes 60% of requests in under 2 hours compared to zero via traditional phone/fax methods, saving up to $449 million industry-wide.
- Predictive analytics for patient risk stratification can save $8,000-$12,000 per avoided readmission t, though real-world results show mixed outcomes with the majority reporting no utilization changes.
- Revenue cycle management optimization reduces administrative workload by 30-60% and denial rates by 20-40% while accelerating cash realization by up to 50% through intelligent automation.
The most successful healthcare organizations start with one high-impact use case like documentation or billing, measure results rigorously, then expand systematically rather than deploying AI across all workflows simultaneously. Success depends on matching specific organizational pain points with appropriate AI technology that addresses current administrative burdens.
 Software development for healthcare has hit a critical milestone: 70% of organizations are now using AI, up from 63% in 2024. The financial effect is compelling, and 85% of executives report AI is helping increase revenue, while 80% see reduced costs. AI-powered healthcare solutions are delivering measurable returns. Predictive analytics healthcare systems save $70,000 to $120,000 per stroke patient. We’ve identified 12 custom software development for healthcare use cases, healthcare workflow automation applications that are changing clinical operations and delivering proven ROI.
Software development for healthcare has hit a critical milestone: 70% of organizations are now using AI, up from 63% in 2024. The financial effect is compelling, and 85% of executives report AI is helping increase revenue, while 80% see reduced costs. AI-powered healthcare solutions are delivering measurable returns. Predictive analytics healthcare systems save $70,000 to $120,000 per stroke patient. We’ve identified 12 custom software development for healthcare use cases, healthcare workflow automation applications that are changing clinical operations and delivering proven ROI.
AI-Powered Clinical Documentation and Ambient Listening Software
“In 2026 we will see AI shift from isolated pilot programs to full enterprise-scale deployment, driven by clearer return on investment. The most visible and prominent example of this will be ambient listening, which will become more of a standard, ubiquitous tool for reducing the burden of clinical documentation.”
— Ben Sharfe, EVP for AI, Altera Digital Health, AI executive in health tech
What This Use Case Solves
Physicians spend over 50% of their workday typing at computers and steal time from direct patient care. The documentation burden has reached a breaking point. About 82.8% of clinicians spend time documenting outside clinical hours on a regular basis, and 75.2% report burnout risk due to documentation alone. Ambient AI listening software addresses this problem. It records physician-patient conversations passively and generates structured clinical notes in the EHR without manual input. The technology transforms documentation from active data entry to the quickest review method. Clinicians can maintain eye contact and participate fully during visits instead of dividing attention between patient and keyboard.
Technical Implementation in Software Development
Custom software development for healthcare that integrates ambient AI requires natural language processing engines. These engines understand medical terminology and context. The systems record visit audio through phone-based apps or desktop interfaces with patient consent. They then analyze conversations using speech recognition and generative AI to produce SOAP notes, problem lists, and after-visit summaries. Deep EHR integration proves critical for sustained value. Bi-directional connections allow the AI to pull patient history for context while pushing completed notes, orders, and billing codes into Epic, Oracle Health, athenahealth, or MEDITECH systems. Human oversight remains non-negotiable. Clinicians review and edit AI-generated notes before finalization to catch hallucinations, omissions, and fabricated information that pose safety risks.
Proven ROI and Time Savings
Healthcare workflow automation through ambient AI delivers measurable financial returns. Physicians using these tools saw a 5.8% increase in weekly relative value units and 2.8% more encounters per week. This translates to about $300,000 per physician each year based on 2025 Medicare rates. Riverside Health reported a 14% increase in HCC diagnoses documented per encounter and an 11% boost in work RVUs after deploying Abridge. Time savings range from 2 minutes per appointment at the Cleveland Clinic to 30 minutes per day at UW Health. Burnout scores dropped from 50.6% to 29.4% in 42 days at Mass General Brigham. Subscription costs run $200 to $600 per clinician each month.
Real-Life Healthcare Application
Cleveland Clinic deployed Ambience Healthcare’s AI Scribe to more than 4,000 physicians and advanced practice providers. The system documented 1 million patient encounters with 76% adoption for scheduled office visits. UW Health’s randomized trial with Abridge reduced documentation time by 30 minutes per day and improved diagnosis billing accuracy before rolling out to 800 providers in Wisconsin and Illinois. Nearly two-thirds of hospitals using Epic Systems have adopted ambient AI tools as the EHR giant now offers built-in charting functionality.
Predictive Analytics Healthcare Solutions for Patient Risk Stratification
What This Use Case Solves
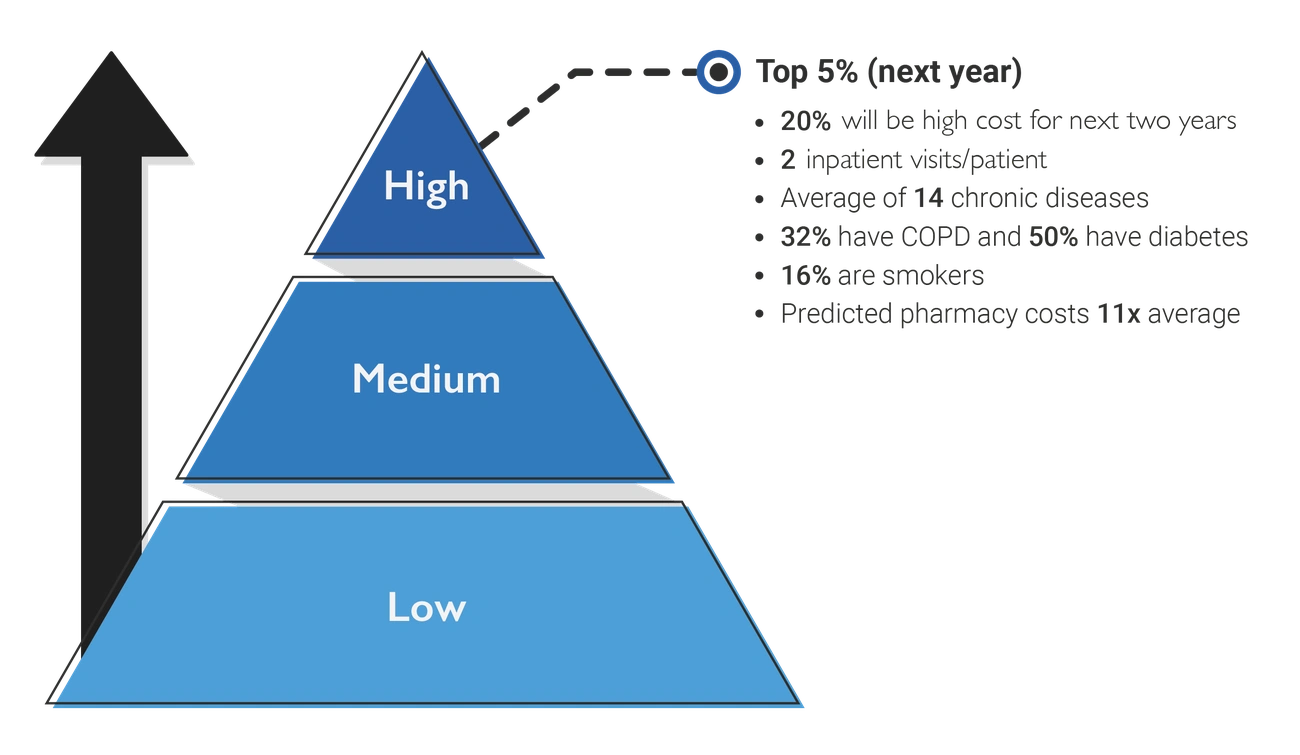
Risk stratification software identifies patients most likely to experience hospital admissions, emergency department visits, or disease progression before these costly events occur. Custom software development for healthcare uses predictive analytics, healthcare models, and categorizes populations into low, medium, and high-risk groups based on clinical factors, utilization patterns, and social determinants. High-risk individuals typically comprise a small percentage of the total population. Medium-risk accounts for 35% and low-risk accounts for 60%. The software wants to target preventive interventions toward those who will benefit most and move care from reactive to proactive management. But ground evaluations reveal mixed outcomes. Research that analyzed 51 studies found that the majority reported no change or most significant increases in healthcare utilization within targeted groups, with only one-third demonstrating benefit.
Technical Implementation in Software Development
Predictive analytics healthcare solutions rely on three commonly adopted models. The Adjusted Clinical Groups system from Johns Hopkins uses diagnoses, age, gender, and classifies patients into 93 categories. It achieves C-values of 0.67 for emergency department predictions and 0.76 for cost predictions. The Charlson Comorbidity Index categorizes populations into six groups based on comorbidities and chronic conditions. Hierarchical Condition Categories, designed by Medicare, uses demographic data and ICD-10 codes and assigns individualized risk scores across 70 condition categories. AI-powered healthcare implementations use natural language processing to extract insights from unstructured clinical notes, integrate disparate data from EHRs and health information exchanges, and generate immediate predictions at the point of care. Neural network models have achieved 97.5% accuracy in predicting CPT codes from pathology reports.
Proven ROI and Time Savings
Organizations using AI for prospective risk adjustment could generate savings up to $360 billion annually across health plans. Providers that implemented healthcare workflow automation through risk stratification experienced a 25% relative decrease in readmission rates. One Blue Cross Blue Shield plan achieved a 40% increase in value per chart by improving HCC coding. Heart failure readmission prevention saves $8,000 to $12,000 per avoided readmission and returns $600,000 to $1.2 million annually for systems treating 300 patients. A Danish study using AI-based risk prediction in colorectal cancer surgery reduced complications from 28% to 19.1% while proving cost-effective.
Real-World Healthcare Application
UC San Diego Health deployed a deep learning sepsis prediction platform that achieved 99.44% uptime with zero hours of system downtime across emergency departments. The Danish colorectal cancer registry developed an AI model on 18,403 patients that reduced medical complications from 37.3% to 23.7% when individual-specific treatment followed risk predictions. Notwithstanding that, 86% of implemented prediction models carry a high risk of bias. Only 32% were assessed for calibration during development, and 27% received external validation.
Automated Medical Coding and Billing Systems
What This Use Case Solves
Manual medical coding creates financial hemorrhaging for healthcare organizations of all sizes. Research shows 80% of U.S. medical bills contain errors and cost Americans $210 billion each year. Coding mistakes account for 42% of Medicare claim denials. Coding errors cost the healthcare system approximately $36 billion annually. Custom software development for healthcare using AI-driven natural language processing automates code assignment from clinical documentation. This reduces manual effort and improves accuracy. These systems analyze physician notes and extract diagnoses and procedures, then suggest appropriate ICD-10, CPT, and HCPCS codes. Claim scrubbing functionality identifies and corrects errors before submission. This prevents denials that trigger costly rework cycles.
Technical Implementation in Software Development
Healthcare workflow automation for coding relies on NLP engines trained on medical terminology and historical coding patterns specific to each organization. The software integrates bi-directionally with EHR systems through HL7, FHIR, and X12 protocols. It pulls clinical documentation while pushing verified codes into billing workflows. AI-powered healthcare platforms offer both autonomous and semi-autonomous modes. Autonomous systems handle routine cases without human intervention and achieve 95% accuracy rates. Complex cases are routed to human coders to review. Rule-based engines verify code combinations against National Correct Coding Initiative edits, check Medical Necessity edits, and apply payer-specific requirements before claim generation.
Proven ROI and Time Savings
Organizations that implement automated coding report coder productivity increases of 20% to 72%. Auburn Community Hospital experienced a 50% reduction in discharged-not-final-billed cases, over 40% increase in coder productivity, and 4.6% rise in case mix index. A Fresno community health network reduced prior-authorization denials by 22% and services-not-covered denials by 18%. This saved 30 to 35 hours each week. MediMobile’s Genesis platform increases annual revenue by $30,000 to $50,000 per physician while reducing claim denials by 50% and coder workload by 75%. Clients see ROI in one to three months.
Ground Healthcare Application
Banner Health automates insurance coverage discovery using AI bots that blend patient information across financial systems and generate appeal letters based on denial codes. Healthcare organizations report 30% to 50% reductions in coding-related audit findings after they implement automation tools. Organizations can expect 95% autonomous coding rates for routine cases by 2027.
AI-Driven Prior Authorization Automation

What This Use Case Solves
Doctors and staff invest 13 hours per week managing prior authorizations. 94% of physicians report that these approvals delay patient care. The process functions as a payer requirement where providers must get preapproval before administering services or medications as a condition of coverage. Prior authorization wants to prevent inappropriate service utilization and verify that first-line treatments are attempted before escalating to more invasive therapies. Manual workflows involve gathering documentation, navigating payer-specific portals, and tracking approvals through phone calls and faxes. 93% of patients experience care delays, and 82% sometimes abandon treatment due to these barriers. Custom software development for healthcare using AI automation targets this administrative bottleneck and streamlines the workflow from eligibility detection through appeals.
Technical Implementation in Software Development
AI-powered healthcare platforms for prior authorization deploy triage engines that classify request complexity using member eligibility data, clinical claims history, and EHR elements. Natural language processing extracts structured information from benefits documentation and unstructured clinical notes combined from multiple sources. Classification algorithms then provide likelihood scores for different outcomes and apply automated eligibility determination, clinical rationale based on historical decisions, and provider utilization profiles. Healthcare workflow automation reduces workflow steps through dynamic rules lined up with complexity levels. CMS requires impacted payers to build FHIR APIs beginning in 2026. These APIs enable providers to determine PA requirements and submit requests electronically, with decisions delivered within 72 hours for accelerated cases and seven days for standard requests.
Proven ROI and Time Savings
Organizations implementing prior authorization automation achieve 50% to 75% reduction in manual tasks. Innovaccer projects 50% reduction in clinician time, twofold staff productivity gains, and 5x ROI through efficiency improvements and reduced denials. Cohere reports 47% reduction in administrative costs while automating up to 90% of prior authorizations. Electronic prior authorization delivers over 60% of requests in under two hours compared to zero via phone or fax. Availity AuthAI renders recommendations in under 90 seconds on average. The healthcare industry could save $437 million to $449 million annually through PA digitization. Automated authorizations cost $0.04 compared to $3.68 for manual processing.
Ground Healthcare Application
Blue Cross Blue Shield of Massachusetts employs AI tools to extract relevant health record data and reduce provider burden. Cohere’s platform has processed over 15 million authorizations with 99% of requests submitted, including clinical data. The platform achieved 95% reduction in appeals and grievances. Fort HealthCare achieved 91% successful submission rates with 15 minutes saved per authorization. Care New England avoided hiring 14 additional staff members and achieved 55% reduction in authorization-related write-offs. The organization saved 2,841 staff hours through automation. MUSC Health reports 35% to 45% touchless submission rates for in-scope authorizations.
Intelligent Appointment Scheduling and Patient Access Software
What This Use Case Solves
Scheduling requests represent the most common inbound call type at healthcare organizations and account for 19% of phone volume. Healthcare call centers handle an average of 2,000 calls daily. Peak staffing meets only 60% of the required coverage and results in 7% abandon rates that translate to $45,000 in daily revenue loss. Each scheduling call averages 4 minutes, including preparation, handling, dispositioning, and documentation. No-shows cost the United States around $150 billion each year. Custom software development for healthcare using AI-powered healthcare scheduling addresses these inefficiencies through predictive analytics healthcare models that forecast cancellations and conversational agents that handle routine requests on their own. These systems use intelligent matching algorithms that connect patients with appropriate providers based on clinical needs, availability, and insurance networks.
Technical Implementation in Software Development
Healthcare workflow automation platforms deploy conversational AI agents that verify patient identity using date of birth and cancel or reschedule visits. These agents write notes directly into patient charts. Predictive Scheduler technologies use AI to forecast patient demand and prioritize appointments based on urgency. The systems adjust schedules automatically with up-to-the-minute data. They integrate with EHRs through FHIR APIs and pull scheduling rules while pushing completed bookings. Amazon Bedrock AgentCore coordinates specialized agents for eligibility verification, appointment scheduling, and reminders while maintaining HIPAA compliance. Multi-channel access provides patients with web portals, mobile apps, and SMS for 24/7 self-scheduling.
Proven ROI and Time Savings
Organizations that implement intelligent scheduling report 300% ROI. A 20-site provider reduced no-shows by 20% and saved 5 minutes per booking to reclaim $1.6 million each year against a $400,000 investment. Pine Park Health returned around 2.1 FTE to medical assistant teams for complex care coordination. Automated text reminders reduce missed appointments by up to 28%. Practices that implement smart scheduling systems achieve 15% to 30% no-show rate reductions. Weill Cornell Medicine increased scheduled appointments by 47%.
Real-Life Healthcare Application
Pine Park Health deployed Ava for appointment reminders and Jay for proactive scheduling. Jay booked visits with 55.7% of connected callers while filling open slots that would otherwise go unused. Four healthcare organizations went live with Epic’s Conversational SMS Scheduling and initiated appointment conversations via text in around 20 seconds.
Medical Imaging Analysis and Diagnostic Support Tools
What This Use Case Solves
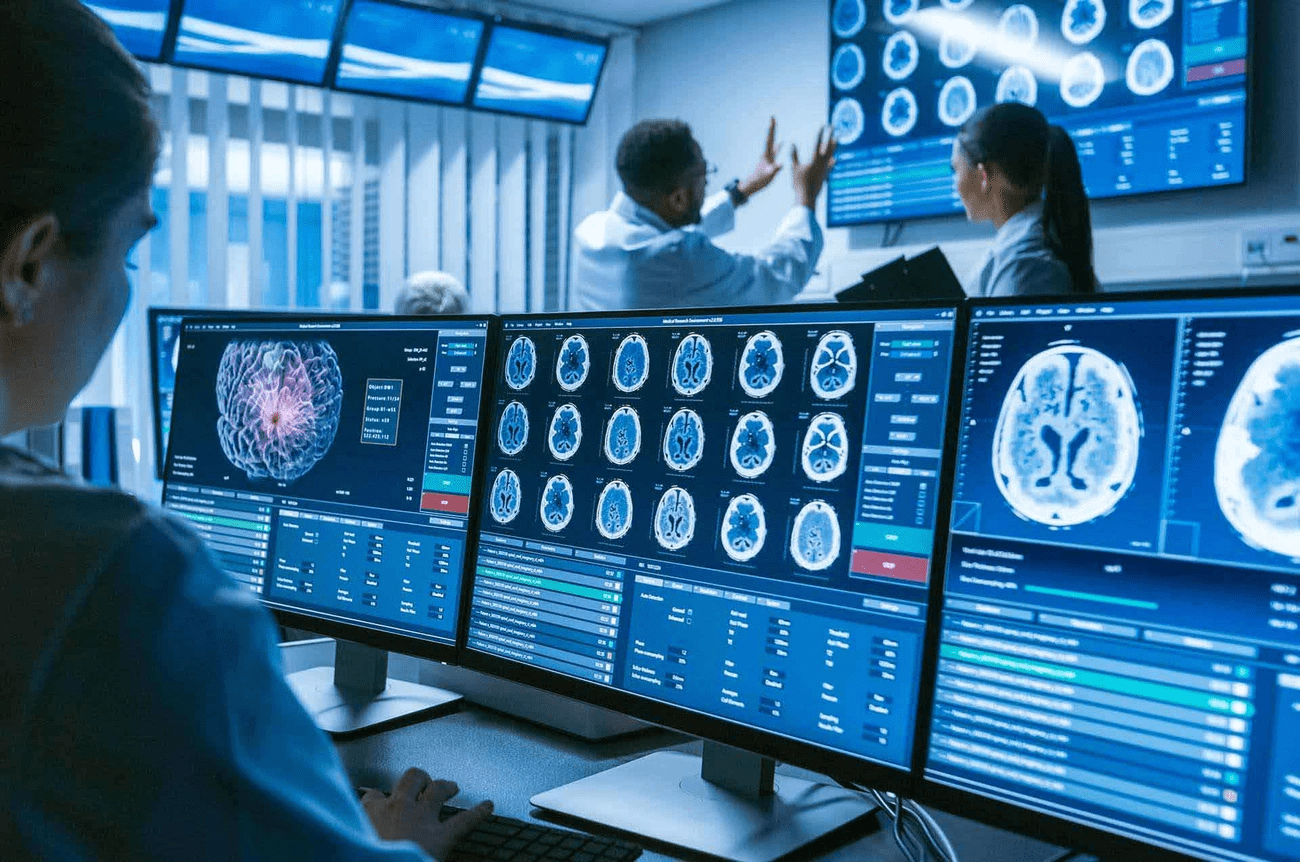
Radiologists’ workload has doubled over two decades. They must analyze hundreds more images daily while facing a 30% to 40% global workforce gap. Custom software development for healthcare using AI-powered healthcare imaging tools addresses the cognitive and administrative burden that slows radiologists down, not just detection capability. AI systems combine findings across multiple exams and summarize patient history. They factor in clinician intent and translate image data into practical reports rather than highlighting lesions. Successful platforms reduce friction between systems instead of adding separate detection overlays that increase cognitive load.
Technical Implementation in Software Development
Healthcare workflow automation for medical imaging relies on convolutional neural networks trained on annotated datasets. These networks perform image segmentation, feature extraction, and classification. Deep learning algorithms analyze CT scans, MRIs, X-rays, and ultrasounds at the pixel level. They detect patterns human eyes miss. The software integrates with PACS and hospital information systems. This enables triage prioritization where algorithms flag urgent cases like intracranial hemorrhages immediately. Platforms must support local validation and tuning. They need to adapt to specific practice patterns rather than deploying inflexible standalone models.
Proven ROI and Time Savings
Organizations using AI for medical imaging report 57% achieving measurable ROI. Massachusetts General Hospital reduced mammography false positives by 30% using triage tools. AI reconstructs high-quality images with 80% lower radiation dose and 85% less noise. A UCLA computer model reduced processing time by a factor of 5,000 while matching clinical specialist accuracy. MRI algorithms deliver scans up to 86% faster. Deep learning achieves 93.2% AUC in detecting gliomas and 89.6% for breast cancer.
Real-Life Healthcare Application
St. Luke’s Health System implemented BoneView AI across its entire network after seven years of gradual radiology AI integration. The system addresses workflow issues and staffing shortages. University Hospitals launched RadiCLE to work with global startups. They are developing fracture and stroke detection algorithms.
Healthcare Workflow Automation for Care Coordination
What This Use Case Solves
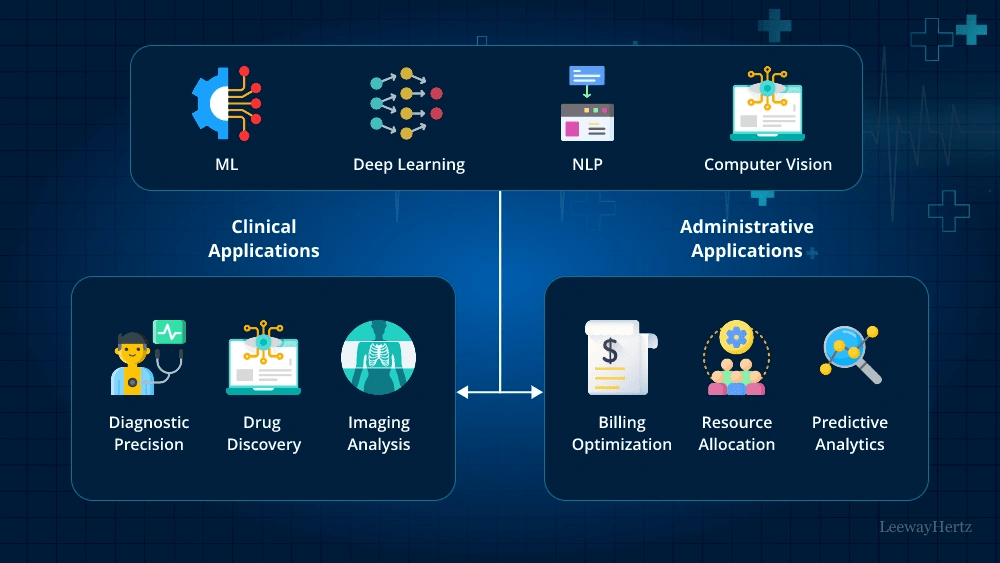
Fragmented care coordination workflows prevent care teams from seeing complete patient views in a variety of EHR systems. Care managers juggle large caseloads without tools to identify patients for care management programs or track care plan tasks. Missed patient identification affects care quality and drives up total costs. Custom software development for healthcare using AI-powered healthcare platforms addresses these gaps through automated workflows that trigger on specific events, predictive risk models that prioritize high-need patients, and unified data views that connect medical, behavioral, and social care teams.
Technical Implementation in Software Development
Healthcare workflow automation platforms deploy case enrichment algorithms that trigger when patients are discharged. The algorithms check against care program routing decision trees and execute automated tasks without human intervention. Predictive analytics healthcare models use evidence-based algorithms and clinical pathways to follow patients across the entire care continuum. The systems integrate with EHRs through FHIR connectors and pull detailed longitudinal patient data while pushing care plans, appointments, and notifications directly into provider workflows. Natural language processing extracts insights from clinical documentation to auto-populate care protocols and assessments.
Proven ROI and Time Savings
Organizations that implement care coordination automation report 65% reduction in all-cause 30-day readmission rates and 85% reduction in provider workload. Care managers reduce documentation time from 4.5 hours to less than 1 hour daily. A skilled nursing facility decreased readmissions from 19% to 13% and saved 420 staff hours monthly. The facility achieved 89% first-year ROI against a $36,000 investment. Another organization projected $350,000 in annual savings with 7% care gap closure rate increase. Behavioral health providers using ambient documentation achieved 70% reduction in paperwork time.
Ground Application
Arcadia Care Manager combines predictive risk models with automated workflows and triggers follow-up text messages and care manager appointments within 48 hours post-discharge. The system notifies primary care physicians for seven-day follow-ups. WellSky’s CarePort platform helps with over 30% of annual hospital discharges to post-acute providers in the United States. Clients experience 11% readmission reductions.
Drug Discovery and Development Acceleration Software
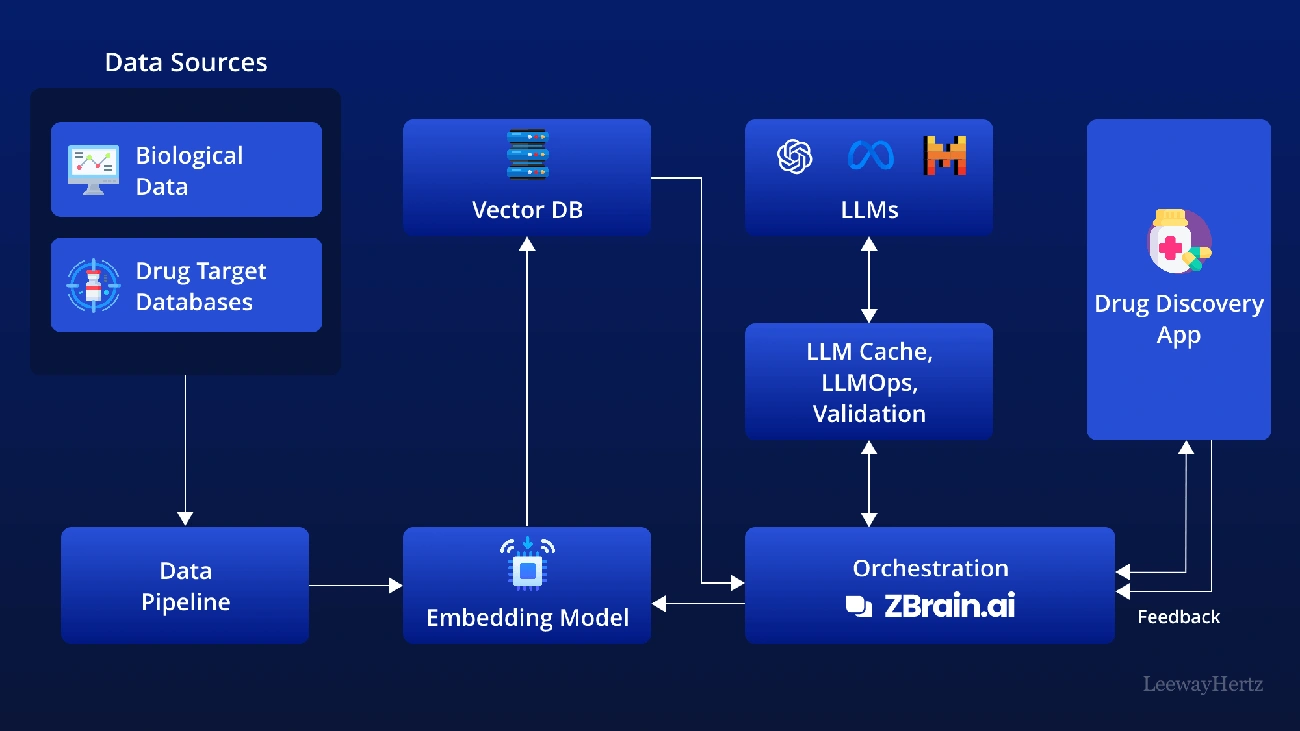
What This Use Case Solves
Traditional drug development requires 10 to 17 years and costs between $100 million and $2.8 billion per approved drug. Only 5% of candidates passing Phase I trials reach the market. The situation gets worse: 90% of drug candidates fail in preclinical or clinical trials. Custom software development for healthcare using AI addresses this problem. The technology analyzes vast biological and chemical data during compound identification. It predicts efficacy and toxicity before synthesis and optimizes clinical trial design. The technology removes uncertainty from molecular target identification and lead compound optimization. This dramatically improves the chances of identifying commercially viable candidates while reducing both costs and timelines.
Technical Implementation in Software Development
AI-powered healthcare platforms for drug discovery deploy generative adversarial networks and deep neural networks to design novel molecules. Natural language processing extracts scientific knowledge from patents, publications, and trial data. This accelerates manual target assessments by over 30%. Foundational chemistry models map millions of chemical compounds by structure and function. They predict ADME properties, toxicity, and bioactivity before laboratory testing. AlphaFold and ESMFold predict protein structures in seconds, enabling rapid compound design. Reinforcement learning optimizes molecules iteratively. Biomedical knowledge graphs aid drug repurposing by simplifying complex biological systems.
Proven ROI and Time Savings
Organizations heavily investing in AI could see ROI increases exceeding 45%. Insilico Medicine identified a fibrosarcoma target and advanced a preclinical candidate in 18 months at approximately $150,000. The traditional approach takes 4 to 6 years. Exscientia designed a Phase I-ready OCD drug in under 12 months compared to the typical 4 to 5 years. AI-guided screening achieves hit rates of 22% to 46% versus 2% random screening. AI-designed small molecules demonstrate 80% to 90% Phase I success rates versus 40% to 65% with traditional methods. McKinsey estimates AI could generate $60 billion to $110 billion in economic value for pharma each year. The technology could cut drug discovery timelines in half.
Ground Healthcare Application
Healx used AI to identify new uses for drug HLX-0201 in treating fragile X syndrome. The drug advanced to Phase II clinical trials within 18 months. Deep Genomics applied its AI platform to identify novel targets and screen oligonucleotide candidates for Wilson’s disease in just 18 months. Insilico Medicine used GENTRL to complete an AI drug discovery challenge in 21 days, generating a highly active DDR1 kinase inhibitor. Genentech deploys a “lab in a loop” strategy where AI models trained on lab and clinical data make predictions tested through experiments. Results retrain models for improved accuracy. Roche works together with AWS and NVIDIA to boost proprietary machine learning algorithms, speeding drug development.
AI-Powered Healthcare Chatbots and Virtual Health Assistants

What This Use Case Solves
Virtual assistants handle routine patient interactions that consume staff capacity. Private practices faced staffing shortages and rising wages before hiring virtual assistants for faxes, messages, and billing tasks. Patients expect on-demand support. Most health systems lack 24/7 availability. Chatbots address appointment scheduling, medication reminders, symptom triage, and chronic disease management at scale. Engagement rates exceed 90% for enrolled patients, with adherence reaching 97% in some implementations. Only half of chronic disease patients follow care plans as instructed.
Technical Implementation in Software Development
Custom software development for healthcare deploys natural language processing and machine learning algorithms to understand medical queries and adapt responses over time. AI-powered healthcare platforms integrate with EHR systems through FHIR APIs. This enables live data access while maintaining HIPAA compliance. Conversational AI allows patients to text questions from phones and receive responses right away. Systems incorporate therapeutic approaches like cognitive behavioral therapy and motivational interviewing.
Proven ROI and Time Savings
Healthcare workflow automation through chatbots saves $3.60 billion around the world. Organizations report 40% operational efficiency improvements. GetWendi chatbot saved hours each day and boosted conversion rates by 40% at Spring Forest Counseling. Virtual assistants reduce administrative costs by 47% while automating up to 90% of prior authorizations. Average handle times drop 20%. This delivers cost benefits of hundreds of thousands of dollars.
Real-Life Healthcare Application
Commure’s Memora Health technology achieves over 90% patient engagement rates. Children’s Healthcare of Atlanta launched an AI chatbot providing digital concierge services through their mobile app. Essentia Health reduced interview scheduling from three days to 28 minutes using a virtual recruiter chatbot. Sunway Medical Center in Malaysia integrated AI chatbots with diagnostic tools. This involves automated patient data collection and preliminary diagnoses.
Sepsis and Patient Deterioration Early Warning Systems

What This Use Case Solves
Up to 5% of hospitalized patients experience clinical deterioration. Delays in care escalation increase both mortality and length of stay. Sepsis affects 1.7 million adults each year in the United States and kills more than 250,000. Traditional scoring systems don’t deal very well with subtle physiological changes that precede adverse events. Custom software development for healthcare using AI-powered healthcare early warning systems addresses this challenge. These systems monitor patient data without interruption and flag deterioration risks hours before traditional methods can.
Technical Implementation in Software Development
Healthcare workflow automation platforms deploy machine learning models trained on historical patient data. These models classify deterioration risk every six hours. AI algorithms analyze vital signs, lab results, nursing documentation patterns, and clinical notes from EHRs. Gradient-boosted models like eCART outperform traditional scores. They provide 11-hour median lead times compared to 1 hour for older systems. Wearable biosensors capture heart rate, respiratory rate, and temperature data without interruption for up-to-the-minute analysis.
Proven ROI and Time Savings
AI-based early warning models reduce in-hospital mortality by 31%. Predictive analytics healthcare systems save $1.5 million to $3 million each year for typical 100-bed hospitals. One implementation achieved 35.6% mortality risk reduction and 7.5% sepsis risk decrease. The Johns Hopkins system detected severe sepsis six hours earlier than traditional methods. Patients became 20% less likely to die.
Ground Healthcare Application
Johns Hopkins deployed their Targeted Real-Time Early Warning System in five hospitals. The system treated 590,000 patients with 4,000+ clinicians and achieved 82% accuracy. Northwell Health’s AI algorithm predicted patient deterioration 17 hours in advance and anticipated 83% of unplanned ICU transfers.
Revenue Cycle Management Optimization Software

“To survive financially, providers are recognizing that AI and automation are essential for driving efficiency and accuracy across the revenue cycle. RCM is uniquely suited for AI because it involves repeatable, pattern-based work, data-intensive analysis, and rules-driven decision-making.”
— Todd Doze, CEO of Janus Health, revenue cycle management expert
What This Use Case Solves
Healthcare organizations allocate $372 billion to administrative complexity. Of this, $39 billion goes to RCM tasks. Manual processes create billing errors, claim denials, and delayed reimbursements that drain financial performance. Custom software development for healthcare using AI-powered healthcare platforms addresses these inefficiencies. The platforms automate insurance verification, claims submission, payment posting, denial management, and collections. The systems identify billing errors before submission and predict denial patterns. They optimize revenue capture across the patient financial cycle.
Technical Implementation in Software Development
Healthcare workflow automation platforms deploy machine learning for denial prediction and natural language processing to extract billing data from clinical documentation. Robotic process automation handles repetitive tasks. The software integrates with EHRs through HL7 and FHIR protocols. It validates claims against millions of payer rules and checks coding compliance. Predictive analytics healthcare engines analyze historical payment patterns. They forecast revenue and flag high-risk claims before submission.
Proven ROI and Time Savings
Organizations implementing RCM automation achieve 30% to 60% reductions in FTE workload and 20% to 40% denial rate. Cash realization speeds up by 40% to 50%. Manual payment posting takes 2.1 minutes per claim. RPA completes it in 2 seconds. An independent New York hospital saved over $1 million using AI for documentation improvement and medical coding. Partial automation could reduce administrative spending by 42%.
Ground Application in Healthcare
Auburn Community Hospital experienced a 50% reduction in discharged-not-final-billed cases. Coder productivity increased by over 40%. A Fresno community health network reduced prior-authorization denials by 22% and services-not-covered denials by 18%. This saved 30 to 35 hours weekly. About 46% of hospitals use AI in RCM operations now, and 74% have implemented some form of revenue cycle automation.
Clinical Decision Support Systems with AI Integration
What This Use Case Solves
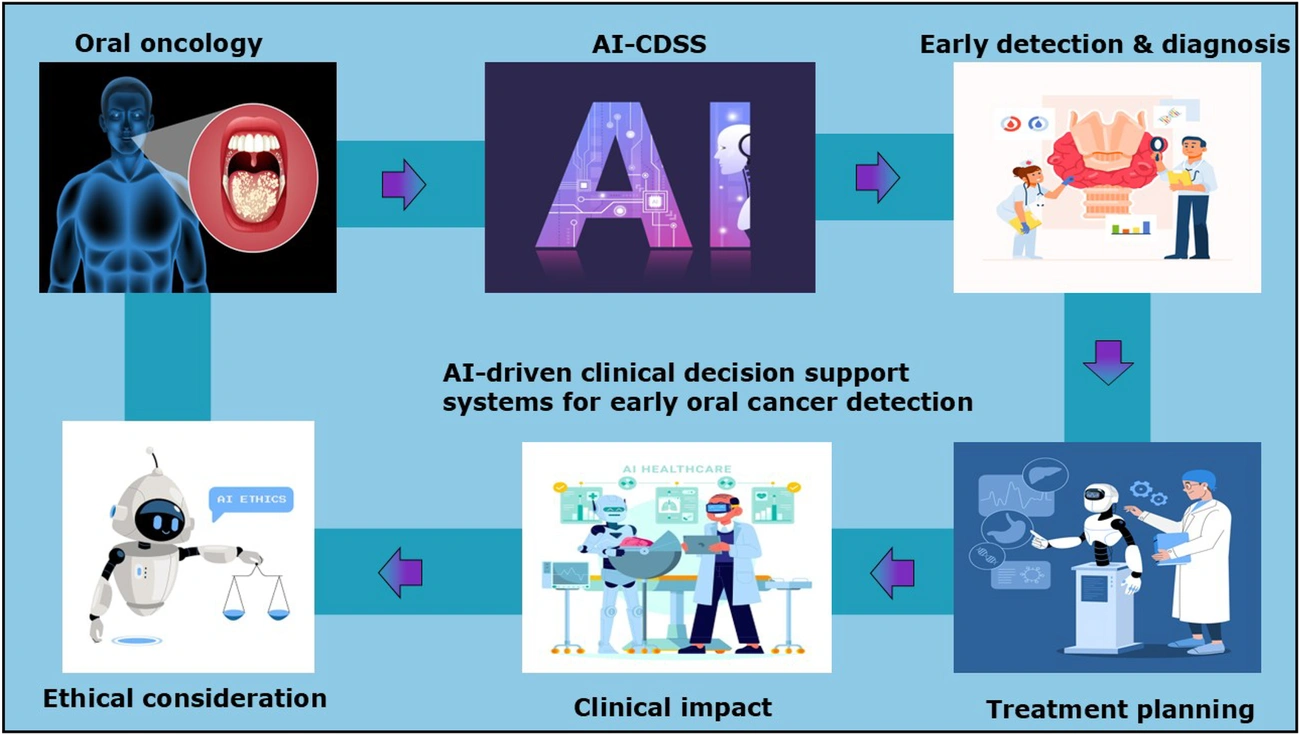
Clinicians face a trust crisis with AI tools. Research shows 41% are aware of colleagues using unauthorized AI applications, while 17% admitted to using unauthorized tools themselves. Custom software development for healthcare addresses this through clinical decision support systems built on peer-reviewed medical evidence rather than open-web data. These platforms blend conflicting research volumes into practical guidance at the point of care and support clinical reasoning without replacing physician judgment. The systems deliver evidence-based treatment recommendations, identify optimal therapies based on patient genetics and history, and flag potential medication interactions before prescribing.
Technical Implementation in Software Development
AI-powered healthcare CDSS platforms deploy machine learning algorithms trained on curated clinical databases to generate customized recommendations. Natural language processing extracts information from unstructured EHR notes and transforms free-text into structured data. Retrieval-augmented generation architecture ensures every output links to validated knowledge sources rather than generating speculative content. Systems like UpToDate Expert AI build on recommendations from over 7,600 clinicians, with every answer including transparent reasoning and direct topic links. The platforms integrate FHIR APIs for immediate patient data access while maintaining strict HIPAA compliance.
Proven ROI and Time Savings
Healthcare workflow automation through CDSS reduces manual documentation tasks, with NLP automating clinical note extraction. Organizations report reduced medical errors through automated alerts for drug interactions and contraindications. Systems identify unnecessary tests and duplicate procedures, decreasing healthcare costs. Hospitals using AI for image analysis saw radiology wait times drop by 50%. Johns Hopkins reduced ICU mortality by 20% using AI-based sepsis detection.
Real-Life Healthcare Application
Nearly two-thirds of physicians now use health AI, representing a 78% increase from the previous year. Up to 80% of hospitals report some AI use in point-of-care workflows. DynaMed employs clinician-in-the-loop approaches and monitors thousands of journals with editorial teams ensuring recommendations remain current and defensible. Notwithstanding that, only three AI-CDSS interventions achieved “highly effective” categorization in systematic reviews, with patient privacy and health equity remaining ongoing concerns.
Medication Management and Prescription Verification Software
What This Use Case Solves
Medication errors occur during prescribing, dispensing, or administering drugs. Up to 50% of all medication mistakes happen at these stages and contribute to 700,000 emergency department visits each year. These prescription errors cost about $3.5 billion per year in the United States. Custom software development for healthcare using AI-powered healthcare platforms prevents up to 80% of these errors. The systems automate prescription translation and verify medications through barcode scanning. They flag drug interactions before reaching patients. Medication reconciliation burdens clinicians. Home health patients average 13 medications and require 20 minutes of manual data entry per patient.
Technical Implementation in Software Development
Healthcare workflow automation deploys natural language processing to translate prescription instructions. This achieves substantially fewer errors than existing systems. Barcode verification systems scan patient, staff, and medication identifiers at three levels. They integrate with electronic medication records. AI platforms like MEDIC reduced near-misses by 33% through prescription-production system integration. The software connects with EHRs via FHIR APIs. It analyzes referral documents and medication bottle photographs to auto-populate patient records.
Proven ROI and Time Savings
Organizations that implement medication management software report 56% reductions in adverse drug reactions and 45% decreases in observed medication errors. WellSky Extract delivers 60% time savings. It reduces medication reconciliation from 20 minutes to 8 minutes per patient. McLean Hospital identified 82 medication errors across 72 patients. 88% of these errors could have caused harm if left uncorrected. Baptist Health saved 7 million clicks after seven months.
Real-Life Healthcare Application
Emory Healthcare achieved 13% improvement in medications imported within 24 hours of admission. AI boosted medication history data by 81%. Sharp HealthCare’s Enhanced Medication Management system reduced schizophrenia cohort readmissions by 8.4%.
Comparison Table: AI Use Cases in Healthcare Software Development
| Use Case | Main Problem Solved | Key ROI Metrics | Time Savings | Implementation Technology | Real-Life Adoption Example |
|---|---|---|---|---|---|
| AI-Powered Clinical Documentation and Ambient Listening Software | Physicians spend over 50% of their workday typing, and 82.8% document outside clinical hours | $300,000 per physician each year; 5.8% increase in weekly RVUs; Burnout scores dropped from 50.6% to 29.4% | 2 to 30 minutes saved per appointment; 30 minutes per day at UW Health | NLP engines with speech recognition and generative AI; Deep EHR integration via bi-directional connections; Human oversight for review | Cleveland Clinic deployed to 4,000+ physicians, documenting 1 million encounters with 76% adoption |
| Predictive Analytics Healthcare Solutions for Patient Risk Stratification | Identifies high-risk patients before costly events occur; Mixed real-life outcomes with the majority showing no change in utilization | Up to $360 billion potential annual savings across health plans; 25% relative decrease in readmission rates; $8,000 to $12,000 saved per avoided heart failure readmission | Not mentioned | Three models: Johns Hopkins ACG system, Charlson Comorbidity Index, Hierarchical Condition Categories; NLP extracts insights from clinical notes; Neural networks achieve 97.5% accuracy | UC San Diego Health deployed a deep learning sepsis platform with 99.44% uptime and zero downtime |
| Automated Medical Coding and Billing Systems | 80% of U.S. medical bills contain errors costing $210 billion each year; Coding mistakes account for 42% of Medicare claim denials | 20% to 72% coder productivity increases; $30,000 to $50,000 annual revenue increase per physician; 50% reduction in claim denials; ROI in 1 to 3 months | 30 to 35 hours saved weekly; Manual posting takes 2.1 minutes vs 2 seconds with automation | NLP engines trained on medical terminology; HL7, FHIR, and X12 protocol integration; 95% accuracy rates for autonomous systems; Rule-based validation engines | Auburn Community Hospital achieved 50% reduction in discharged-not-final-billed cases and 40% productivity increase |
| AI-Driven Prior Authorization Automation | Doctors spend 13 hours per week on prior authorizations; 94% report delays in patient care; 93% of patients experience care delays | 50% to 75% reduction in manual tasks; 5x ROI through efficiency improvements; $437 million to $449 million potential annual industry savings; $0.04 automated cost vs $3.68 manual | Over 60% of requests completed in under 2 hours; Recommendations in under 90 seconds; 15 minutes saved per authorization | Triage engines with classification algorithms; NLP extracts structured information; FHIR APIs for electronic submission; 72-hour expedited and 7-day standard decision delivery | Cohere processed 15 million+ authorizations with 95% reduction in appeals; Care New England saved 2,841 staff hours |
| Intelligent Appointment Scheduling and Patient Access Software | Scheduling requests account for 19% of call volume; 7% abandon rates translate to $45,000 daily revenue loss; No-shows cost $150 billion each year | 300% ROI; $1.6 million annual savings for 20-site provider against $400,000 investment; 20% no-show reduction; 47% increase in scheduled appointments | 5 minutes saved per booking; About 20 seconds to initiate text conversations | Conversational AI agents with identity verification; Predictive Scheduler forecasting demand; FHIR API integration; Multi-channel access (web, mobile, SMS, phone) | Pine Park Health’s Jay booked visits with 55.7% of connected callers; Weill Cornell Medicine increased appointments by 47% |
| Medical Imaging Analysis and Diagnostic Support Tools | Radiologists’ workload doubled over two decades; 30% to 40% global workforce gap | 57% achieving measurable ROI; 30% reduction in mammography false positives; 80% lower radiation dose with 85% less noise | Processing time reduced by a factor of 5,000; MRI scans up to 86% faster | Convolutional neural networks for image segmentation; Deep learning algorithms analyze at the pixel level; Direct PACS and HIS integration; Real-time triage prioritization | St. Luke’s Health System implemented BoneView AI network-wide after 7 years of gradual integration |
| Healthcare Workflow Automation for Care Coordination | Fragmented care coordination prevents complete patient views; Care managers lack tools to identify patients for programs efficiently | 65% reduction in 30-day readmissions; 85% reduction in provider workload; 89% first-year ROI; $350,000 projected annual savings | Documentation time reduced from 4.5 hours to less than 1 hour daily; 420 staff hours saved monthly | Case enrichment algorithms with automated triggers; FHIR connectors for EHR integration; NLP extracts insights from clinical documentation; Predictive risk models | Arcadia Care Manager triggers follow-ups within 48 hours post-discharge; WellSky CarePort handles 30%+ of annual U.S. hospital discharges |
| Drug Discovery and Development Acceleration Software | Traditional development takes 10 to 17 years and costs $100 million to $2.8 billion; 90% of candidates fail in trials | ROI increases exceeding 45% for heavy AI investors; $60 billion to $110 billion potential annual economic value; 80% to 90% Phase I success rates vs 40% to 65% traditionally | Development timelines cut in half; 18 months vs 4 to 6 years traditionally; 12 months vs 4 to 5 years for Phase I-ready drugs | Generative adversarial networks and deep neural networks; NLP extracts knowledge from publications; AlphaFold predicts protein structures; Reinforcement learning optimizes molecules | Insilico Medicine identified a target and advanced a candidate in 18 months at $150,000; Exscientia designed a Phase I-ready drug in under 12 months |
| AI-Powered Healthcare Chatbots and Virtual Health Assistants | Routine patient interactions consume staff capacity; Most health systems lack 24/7 availability; Only half of chronic disease patients follow care plans | $3.60 billion saved globally; 40% operational efficiency improvements; 40% conversion rate boost; 47% administrative cost reduction | Average handle times drop 20%; Interview scheduling reduced from 3 days to 28 minutes | NLP and machine learning algorithms; FHIR API integration with EHRs; Conversational AI for text-based queries; Therapeutic approaches like CBT integration | Commure’s Memora Health achieves 90%+ patient engagement rates; Essentia Health reduced scheduling from 3 days to 28 minutes |
| Sepsis and Patient Deterioration Early Warning Systems | Clinical deterioration occurs in up to 5% of hospitalized patients; Sepsis affects 1.7 million adults each year, killing 250,000+ | 31% reduction in in-hospital mortality; $1.5 million to $3 million annual savings for 100-bed hospitals; 35.6% mortality risk reduction | 11-hour median lead time vs 1 hour for traditional systems; Detection nearly 6 hours earlier than traditional methods | Machine learning models classify risk every 6 hours; Gradient-boosted models like eCART; Wearable biosensors for continuous monitoring; EHR data analysis | Johns Hopkins deployed across 5 hospitals, treating 590,000 patients with 82% accuracy; Northwell Health predicted deterioration 17 hours in advance |
| Revenue Cycle Management Optimization Software | Healthcare allocates $372 billion to administrative complexity, with $39 billion on RCM tasks specifically | 30% to 60% FTE workload reductions; 20% to 40% denial rate decreases; 40% to 50% faster cash realization; Over $1 million saved; 42% potential administrative spending reduction | Manual payment posting: 2.1 minutes vs 2 seconds with RPA; 30 to 35 hours saved weekly | Machine learning for denial prediction; NLP extracts billing data; RPA handles repetitive tasks; HL7 and FHIR protocol integration | Auburn Community Hospital: 50% reduction in discharged-not-final-billed cases; 46% of hospitals currently use AI in RCM |
| Clinical Decision Support Systems with AI Integration | 41% of clinicians are aware of colleagues using unauthorized AI; Trust crisis with AI tools in clinical settings | Reduced medical errors through automated alerts; 50% reduction in radiology wait times; 20% ICU mortality reduction | Not mentioned | Machine learning on curated clinical databases; NLP extracts insights from unstructured notes; Retrieval-augmented generation architecture; FHIR APIs for real-time data | Nearly two-thirds of physicians now use health AI (78% increase); Up to 80% of hospitals report AI use in point-of-care workflows |
| Medication Management and Prescription Verification Software | Up to 50% of medication errors occur during prescribing and dispensing; 700,000 annual ED visits; $3.5 billion annual cost | 56% reduction in adverse drug reactions; 45% decrease in observed medication errors; 60% time savings; AI prevents up to 80% of errors | Medication reconciliation was reduced from 20 minutes to 8 minutes per patient | NLP translates prescription instructions; Barcode verification at three levels; FHIR API integration; Analyzes referral documents and medication photos | Emory Healthcare achieved 13% improvement in medications imported within 24 hours; Sharp HealthCare reduced readmissions by 8.4% |
Conclusion
These 12 use cases demonstrate AI’s transformation from experimental technology to revenue-generating infrastructure in healthcare organizations of all sizes. The data tells a compelling story: documented ROI ranging from reduced claim denials to prevented readmissions, with implementations saving millions annually.
Note that not every AI solution will deliver similar results for your organization. Your success depends on matching specific pain points with appropriate technology, especially when you focus on workflows where administrative burden currently drains resources.
I recommend starting with one high-impact area like clinical documentation or prior authorization. Measure results and then expand systematically. Organizations achieving the strongest returns took this methodical approach rather than deploying AI everywhere at once.
FAQs
How much time can AI-powered clinical documentation tools save physicians?
AI-powered ambient listening software can save physicians between 2 and 30 minutes per appointment, depending on the implementation. Some healthcare systems report up to 30 minutes saved daily in documentation time. These tools work by passively recording physician-patient conversations and automatically generating structured clinical notes, allowing doctors to focus on patient care rather than typing.
What is the typical return on investment for automated medical coding systems?
Automated medical coding systems typically deliver ROI within 1 to 3 months of implementation. Organizations report coder productivity increases of 20% to 72%, annual revenue increases of $30,000 to $50,000 per physician, and up to 50% reduction in claim denials. The systems achieve 95% accuracy rates for routine cases while significantly reducing coding-related audit findings.
How effective are AI early warning systems at preventing sepsis deaths?
AI-based early warning systems for sepsis detection can reduce in-hospital mortality by 31%. These systems detect severe sepsis nearly six hours earlier than traditional methods, making patients approximately 20% less likely to die. For a typical 100-bed hospital, predictive analytics for sepsis and patient deterioration can save between $1.5 million and $3 million annually.
Can AI really reduce prior authorization processing time?
Yes, AI-driven prior authorization automation can deliver over 60% of requests in under two hours, compared to zero via traditional phone or fax methods. Some platforms render recommendations in under 90 seconds on average, saving approximately 15 minutes per authorization. Organizations implementing these systems report 50% to 75% reduction in manual tasks and up to 5x ROI through efficiency improvements.
What cost savings can healthcare organizations expect from AI chatbots and virtual assistants?
AI-powered healthcare chatbots and virtual health assistants save approximately $3.60 billion globally. Individual organizations report 40% operational efficiency improvements, 40% increases in conversion rates, and 47% reductions in administrative costs. These systems can automate up to 90% of routine tasks like appointment scheduling, medication reminders, and basic patient inquiries while providing 24/7 availability.

